Introduction
A swallowing disorder (dysphagia) is characterized by difficulty or discomfort in swallowing. The difficulty typically arises while ingesting foods and/or liquids. Swallowing disorders following stroke are common, affecting 22% to 65% of patients, and may persist for many months. Swallowing disorders require immediate attention and if ignored may result in serious morbidity or even mortality, especially when identified in patients with acute stroke.
Ramsey D.J.C., Smithard D.G., Kalra L. (2003). Early Assessments of Dysphagia and Aspiration Risk in Acute Stroke Patients. Stroke. 34;1252-1257.
Patient/Family Information
Authors*: Rosemary Martino, MSc PhD; Katie Sharpe MHSc (student)
What is a swallowing disorder?
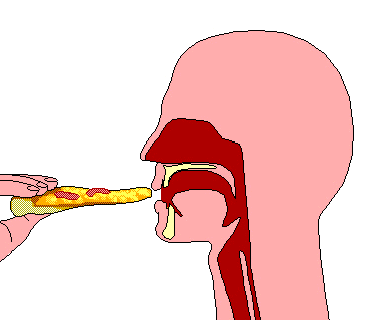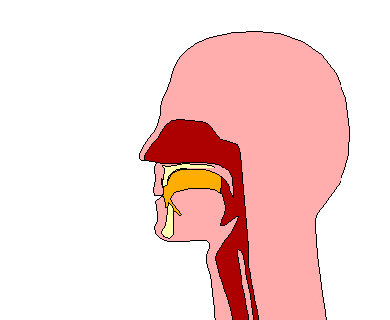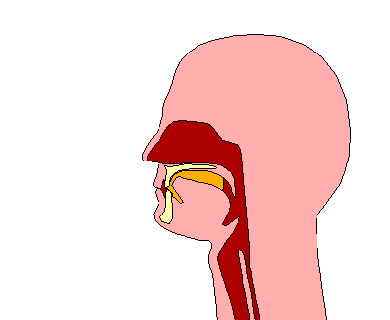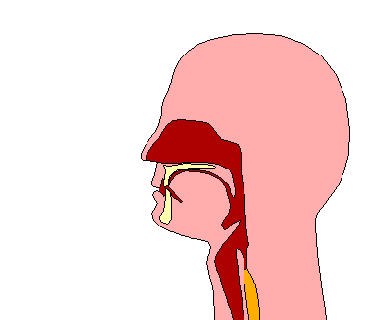
A swallowing disorder (also called dysphagia) is difficulty or discomfort in swallowing. As a result, it can be difficult to eat and drink. When eating, food is placed in the mouth and is then chewed with the teeth to form a compact ball or bolus. Once the bolus of food is formed, the tongue moves the bolus to the back of the mouth. At this point, the swallow is automatically triggered by the brain. The muscles of the back of the tongue and the throat (also called pharynx) squeeze to move the bolus of food through the pharynx and down a tube called the “esophagus”. At the end of the tube, the bolus reaches the stomach. Drinking liquids is very similar to eating foods. The main difference is that when drinking liquids, a bolus of liquid is formed without the need to chew. During both drinking and eating, an important step in swallowing is the automatic closure of the airway or windpipe when the bolus passes through the throat. This closure of the airway prevents food or liquid from going into your lungs. Swallowing difficulties can occur at any point along the swallow, from when the food or drink enters the mouth, to when the bolus passes through the esophagus and into the stomach. The following are examples of common swallowing difficulties along different points of the swallow:
- In the mouth:

- If the lips are not able to close firmly, the food or liquid may drool from the mouth.
- If the tongue is unable to move around the mouth, there may be food left in the mouth after the swallow.
- In the throat:

- If the airway to your lungs is not closed off tightly, food or liquid may accidentally spill into the lungs. This is referred to as “aspiration”. Extended amounts of aspiration can cause a lung infection, such as pneumonia.
- If the muscles of the throat are unable to squeeze the bolus (food or liquid) down into the esophagus, there may be food or liquid left over in the throat after the swallow.
- In the esophagus:

- If the muscles at the top of the esophagus are weak, food may come back up from the esophagus to the throat. This will cause food to remain in the throat after the swallow.
- If the muscles at the bottom of the esophagus are weak, food may come back up from the stomach. This may create pain in the chest and/or a bad acidic taste in the mouth.
How frequent are swallowing disorders?
Swallowing disorders following a stroke are common. Approximately 55% of people who have a stroke have swallowing difficulties during the first days and weeks. Many people regain their swallowing ability within the first month after the stroke. However, around three months after a stroke, as many as 35% of people still have some swallowing difficulties.
What causes swallowing disorders after a stroke?
Swallowing difficulties are caused by damage to the brain. The specific swallowing difficulties vary according to the specific area of the brain affected.
- If the area of the brain that controls muscle movements is affected, then it may be difficult to trigger the muscles of the lips, cheek, tongue, throat, or esophagus to move the bolus. If the area of the brain that controls sensation is affected, then it may be difficult to taste flavors, feel different textures, or identify the temperature of foods or drinks.
- Certain medications that treat important illnesses may also cause swallowing difficulties. For example, some medications may decrease saliva production thereby creating a dry mouth. If the mouth is dry, it is very difficult to form a bolus of food.
- The lack of teeth may also cause swallowing difficulties. For example, loose dentures make it difficult to chew foods.
- Inability to move the hand or fingers after a stroke may cause difficulties in directing food or liquid to the mouth for swallowing.
Can swallowing disorders caused by a stroke be treated?
Yes. In most cases, swallowing disorders can be treated or at least managed. There are a variety of helpful strategies and procedures depending on the cause of the problem. These include behavioural interventions (described below), use of special devices such as spill-proof cups or spoons, medications, and surgery. The information provided here is specific to rehabilitation – and does not include a discussion of surgery or medication. Medication and surgery may be used to treat some swallowing difficulties, and you should discuss this with your physician. There are three main reasons why it is important to treat swallowing difficulties after a stroke:
- to make sure that your nutritional and hydration (liquid intake) requirements are being meet;
- to prevent aspiration-related complications, such as pneumonia;
- to maximize the enjoyment that comes from eating and drinking.
If swallowing difficulties are related to your inability to cut and manage your food because you have difficulty using one hand, specific functional interventions will be needed. For example, you may benefit from specialized utensils to help place foods or liquids in your mouth. Alternatively, assistance with feeding may be necessary by a family member, therapist, or nurse. It is important to know that swallowing problems can be treated or controlled no matter the cause. Don’t be afraid. Talk to your doctor or nurse OR have someone talk to him or her for you. They will be able to help you find the best treatment for your specific problem.
What are behavioural interventions?
Behavioural interventions for swallowing disorders after a stroke include: Safe eating strategies: Self-feeding is strongly encouraged whenever possible. Whether you are an independent eater or you require assistance, there are a number of helpful strategies that can be used to increase swallowing safety:
- if you require eye-glasses, hearing aids, and/or dentures, ensure that you are wearing these at mealtime;
- eat and drink only when you are fully alert;
- sit in an upright position, with your torso at a 90° angle to the ground (pillows can be used to support you);
- eat slowly and allow adequate time for swallowing between bites or sips;
- take small mouthfuls (teaspoon size);
- never combine liquids and solids in the same bite;
- place food on the strong side (the side less effected by the stroke) of the mouth;
- take 2 or more swallows per bite to ensure food is cleared from the mouth and throat;
- try not to talk while chewing or swallowing – save conversation for between bites;
- stay sitting upright for at least 30 minutes after the meal to help food move down into the stomach;
- if you are having swallowing difficulties, it is a good idea to eat while family and other care-givers (nurses, friends who are visiting) are nearby to supervise you and help you eat safely.
Optimum eating environment: An ideal environment for eating is one that is calm with minimal noise and distractions, and has good lighting. Changes in head posture: There are a number of helpful swallowing postures for your head that may be recommended to you. For example, if one side of your throat is weaker than the other, it may help to turn your head towards the weaker side when swallowing, as this directs the food down your stronger side. Changes in the texture or thickness of food and drink: The following are some of the diet textures that may be recommended to you:
- pureed food (e.g., applesauce, yogurt, and mashed potatoes);
- minced or ground food (e.g., meatloaf, shepherd’s pie, and cottage cheese);
- soft or easy to chew food;
- soup and drinks that have been thickened to a nectar-like, honey-like, or pudding-like consistency.
These texture recommendations are usually made following a swallowing assessment performed by a health professional with expertise in swallowing disorders. These recommendations will be discussed with you and your family. Avoidance of certain foods:
- “Dry particulates” or foods that are dry and come in small pieces (e.g., corn, peas, dry rice, noodles, dry cookies, nuts, raisins, hard candies, etc.), as these are difficult to chew;
- Bread products and peanut butter, as these can stick in your throat;
- Spicy and acidic foods (e.g., fried food, coffee, tea, cola, and chocolate), as they promote acid reflux.
Oral muscle exercises: Exercises to strengthen the lips, tongue, and jaw may help to increase your ability to chew and control the movement of food in your mouth. Your therapist should show you these exercises and practice them with you. Swallow maneuvers: There are a number of special maneuvers that can help to improve your swallow. Some maneuvers may not be safe for stroke survivors as they temporarily increase your blood pressure. Ask your speech-language pathologist or other members of your healthcare team if there are any swallow maneuvers appropriate for you. Proper oral hygiene: Ensure that after every meal your mouth is cleaned of all food that may have gotten stuck in your teeth or dentures. Also, your mouth should be kept moist at all times.
Are behavioural interventions effective for swallowing disorders?
Experts have researched the effectiveness of behavioural interventions for swallowing disorders. Some of these studies have shown promising outcomes. Here is a brief overview of what we know:
- Changes in posture: One study looked at patients who aspirated when eating in the upright position. Significant improvement was achieved in some patients by adjusting the position of their head and neck when swallowing. So, as mentioned earlier it may help to turn your head towards the weaker side when swallowing, as this directs the food down your stronger side.
- Changes in the texture or thickness of fluids: Studies have shown that thickening fluids to a honey or milkshake texture may successfully reduce the risk of aspiration, and so, the risk of pneumonia. However, studies have also shown that people placed on a modified texture diet (where your drinks are thickened) have a higher risk of dehydration from not taking in enough regular liquids. Therefore, it is critical that a proper swallowing assessment be conducted to determine the need for this treatment.
- Combined Behavioural Strategies: Studies have looked at treatment involving a combination of the strategies we have discussed, including oral muscle exercises, changes in posture, and modified texture diets. The results suggest that this combination is helpful for better and safer swallowing and nutrition.
Clinician Information
Note: When reviewing the findings, it is important to note that they are always made according to randomized clinical trial (RCT) criteria – specifically as compared to a control group. To clarify, if a treatment is “effective” it implies that it is more effective than the control treatment to which it was compared. Non-randomized studies are no longer included when there is sufficient research to indicate strong evidence (level 1a) for an outcome.
There are many interventions pertaining to the treatment of dysphagia following stroke. This module focuses on treatments that include: oral or pharyngeal stimulation, electrical stimulation, tactile-thermal application, olfactory stimulation, biofeedback, lingual exercises and swallowing training. Studies were excluded from the module based on one or a combination of the following criteria: a study that is not a randomized clinical trial (RCT), a RCT where both groups received the same type of treatment with variable intensities between groups, a RCT where the intervention involves a nasogastric (NG) tube feeding and/or percutaneous endoscopic gastrostomy (PEG), a RCT where the intervention is of pharmacological nature, and a RCT where the population is comprised of less than 50% of patients with stroke. Moreover, studies pertaining to compensatory-type of interventions (e.g. texture modification) were excluded from this module.
To date, 27 studies have investigated the effectiveness of remedial-type interventions available to treat those with identified swallowing disorders, including oral electrical stimulation, swallowing exercises, acupuncture and olfactory stimulation. Sixteen studies are high quality RCTs and 11 studies are of fair quality.
Results Table
View results table
Outcomes
Acute phase - Acupuncture
Functional independence
Effective
1b
One high quality RCT (Xia et al., 2016) investigated the effect of acupuncture on functional independence in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive acupuncture + standard swallowing training or standard swallowing training alone. Functional independence was measured by the modified Barthel Index at baseline and at post-treatment (4 weeks). Significant between group differences in functional independence were found at post-treatment, favoring acupuncture with standard swallowing training vs. standard swallowing training alone.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that acupuncture with standard swallowing training is more effective than standard swallowing training alone in improving functional independence in patients with acute stroke and subsequent dysphagia.
Functional severity of dysphagia
Effective
1b
One high quality RCT (Xia et al., 2016) investigated the effect of acupuncture on functional severity of dysphagia in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive acupuncture + standard swallowing training or standard swallowing training alone. Functional severity of dysphagia was measured by the Dysphagia Outcome and Severity Scale at baseline and at post-treatment (4 weeks). Significant between-group differences in functional severity of dysphagia were found at post-treatment, favoring acupuncture with standard swallowing training vs. standard swallowing training alone.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that acupuncture with standard swallowing training is more effective than standard swallowing training alone in improving functional severity of dysphagia in patients with acute stroke and subsequent dysphagia.
Swallowing function
Effective
1b
One high quality RCT (Xia et al., 2016) investigated the effect of acupuncture on swallowing function in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive acupuncture + standard swallowing training or standard swallowing training alone. Swallowing function was measured by the Standardized Swallowing Assessment at baseline and at post-treatment (4 weeks). Significant between-group differences in swallowing function were found at post-treatment, favoring acupuncture with standard swallowing training vs. standard swallowing training alone.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that acupuncture with standard swallowing training is more effective than standard swallowing training alone in improving swallowing function in patients with acute stroke and subsequent dysphagia.
Swallowing related quality of life
Effective
1b
One high quality RCT (Xia et al., 2016) examined the effects of acupuncture on swallowing related quality of life in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive acupuncture + standard swallowing training or standard swallowing training alone. Swallowing related quality of life was measured with the Swallowing Related Quality of Life scale at baseline and at post-treatment (4 weeks). Significant between-group differences in swallowing related quality of life were found at post-treatment, favoring acupuncture with standard swallowing training vs. standard swallowing training group.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that acupuncture with standard swallowing training is more effective than standard swallowing training alone in improving swallowing related quality of life in patients with acute stroke and subsequent dysphagia.
Acute phase - Acupunture & neuromuscular electrical stimulation (NMES)
Swallowing function
Effective
2a
One fair quality RCT (Zhao et al., 2015) investigated the effect of combined acupuncture and neuromuscular electrical stimulation (NMES) on swallowing function in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive acupuncture + NMES or acupuncture alone. Swallowing function was measured by Kubota’s water test at baseline and post-treatment (2 weeks). A significant between-group difference in change in swallowing function from baseline to post-treatment was seen, in favour of acupuncture + NMES vs. acupuncture alone.
Conclusion: There is limited evidence (Level 2a) from 1 fair quality RCT that acupuncture and NMES is more effective than acupuncture alone in improving swallowing function in individuals with acute stroke and subsequent dysphagia.
Acute phase - Oral care
Microbiological growth
Not effective
2a
One fair quality RCT (Chipps et al., 2014) investigated the effect of oral care on growth of Staphylococcus aureus in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive a standardized oral care program (i.e. timed tooth brushing with a battery powered toothbrush, tongue brushing, flossing, mouth rinse, and lip care performed twice daily by trained nurse) or usual oral care as per hospital policy. Growth of S.aureus was measured by a microbiological swab sample test at baseline and at post-treatment (10 days). No significant between-group differences in microbiological growth were found at post-treatment.
Conclusion: There is limited evidence (Level 2a) that a standardized oral care program is not more effective than usual oral care in preventing microbiological growth in patients with acute stroke and subsequent dysphagia.
Nutritional status
Not effective
2a
One fair quality RCT (Chipps et al., 2014) investigated the effect of oral care on nutritional status in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive a standardized oral care program (i.e. timed tooth brushing with a battery powered toothbrush, tongue brushing, flossing, mouth rinse, and lip care performed twice daily by trained nurse) or usual oral care as per hospital policy. Nutritional status was measured by the Functional Oral Intake Scale (FOIS) at baseline and at post-treatment (10 days). No significant between-group differences in nutritional status were found at post-treatment.
Conclusion: There is limited evidence (Level 2a) that a standardized oral care program is not more effective than usual oral care in improving nutritional status in patients with acute stroke and subsequent dysphagia.
Oral cavity health
Not effective
2a
One fair quality RCT (Chipps et al., 2014) investigated the effect of oral care on oral cavity health in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive a standardized oral care program (i.e. timed tooth brushing with a battery powered toothbrush, tongue brushing, flossing, mouth rinse, and lip care performed twice daily by trained nurse) or usual oral care as per hospital policy. Cavity health was measured by the Revised-THROAT at baseline and at post-treatment (10 days). No significant between-group differences in oral cavity health were found at post-treatment.
Conclusion: There is limited evidence (Level 2a) that a standardized oral care program is not more effective than usual oral care in preventing oral cavities in patients with acute stroke and subsequent dysphagia.
Swallowing ability
Not effective
2a
One fair quality RCT (Chipps et al., 2014) investigated the effect of oral care on swallowing ability in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive a standardized oral care program (i.e. timed tooth brushing with a battery powered toothbrush, tongue brushing, flossing, mouth rinse, and lip care performed twice daily by trained nurse) or usual oral care as per hospital policy. Swallowing ability was measured by the Mann Assessment of Swallowing Ability at baseline and at post-treatment (10 days). No significant between-group differences in swallowing ability were found at post-treatment.
Conclusion: There is limited evidence (Level 2a) that a standardized oral care program is not more effective than usual oral care in improving swallowing ability in patients with acute stroke and subsequent dysphagia.
Acute phase - Oral electrical stimulation
Airway protection
Not effective
1b
One high quality RCT (Power et al., 2006) investigated the effect of oral electrical stimulation on airway protection in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low frequency oral electrical stimulation at the faucial pillar or sham stimulation. Airway protection was measured by the Penetration-Aspiration Scale at baseline and at post-treatment (1 session of 60 minutes duration). No significant between-group difference in airway protection was found at post-treatment.
Conclusion: There is moderate evidence (level 1b) from one high quality RCT that oral electrical stimulation is not more effective than a comparison intervention (sham stimulation) in improving airway protection in patients with acute stroke and subsequent dysphagia.
Swallowing timing
Not effective
1b
One high quality RCT (Power et al., 2006) investigated the effect of oral electrical stimulation on swallowing timing in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low frequency oral electrical stimulation at the faucial pillar or sham stimulation. Swallowing timing (oral transit time, pharyngeal transit time, swallow response time, laryngeal closure duration, cricopharyngeal opening duration) was measured by videofluoroscopy at baseline and at post-treatment (1 session of 60 minutes). There were no significant between-group differences in any measure of swallowing timing at post-treatment.
Conclusion: There is moderate evidence (level 1b) from 1 high quality RCT that oral electrical stimulation is not more effective than a comparison intervention (sham oral electrical stimulation) in improving swallowing timing in patients with acute stroke and subsequent dysphagia.
Acute phase - NMES
Airway protection
Not effective
1b
One high quality RCT (Huang et al., 2014) investigated the effect of neuromuscular electrical stimulation (NMES) and traditional swallowing therapy on airway protection in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES + traditional swallowing therapy, NMES alone, or traditional swallowing therapy alone. Airway protection was measured by the Penetration Aspiration Scale at baseline and post-treatment (3 weeks). No significant between-group differences in airway protection were found at post-treatment.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that NMES and traditional swallowing therapy is not more effective than comparison interventions (NMES alone, traditional swallowing therapy alone) in reducing penetration/aspiration in patients with acute stroke and subsequent dysphagia.
Biomechanical swallowing parameters
Effective
2a
One fair quality RCT (Xia et al., 2011) investigated the effect of neuromuscular electrical stimulation (NMES) on biomechanical swallowing parameters in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive NMES + traditional swallowing therapy, NMES alone, or traditional swallowing therapy alone. Biomechanical swallowing parameters were measured by the Videofluoroscopic Swallowing Study (VFSS) at baseline and at post-treatment (4 weeks). Significant between-group differences in biomechanical swallowing parameters were found at post-treatment favoring NMES + traditional swallowing therapy vs. NMES alone, and favouring NMES + traditional swallowing therapy vs. traditional swallowing therapy alone.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that NMES combined with traditional swallowing therapy is more effective than comparison interventions (NMES alone, traditional swallowing therapy alone) in improving biomechanical swallowing parameters in patients with acute stroke and subsequent dysphagia.
Functional oral intake
Effective
2a
Two fair quality RCTs (Woo Lee et al., 2014), Zhang et al., 2016) investigated the effect of neuromuscular electrical stimulation (NMES) on functional oral intake in patients with acute stroke and subsequent dysphagia.
The first fair quality RCT (Woo Lee et al., 2014) randomized patients to receive either NMES sensory approach + traditional swallowing therapy or traditional swallowing therapy alone. Functional oral intake was measured by the Function Oral Intake Scale (FOIS) at baseline, post-treatment (3 weeks) and at follow-up (6 and 12 weeks). Significant between-group differences in functional oral intake were found at all time points, favoring NMES traditional swallowing therapy vs. traditional swallowing therapy alone.
The second fair quality RCT (Zhang et al., 2016) randomized patients to receive NMES sensory approach, NMES motor approach, or no NMES; all groups received traditional swallowing therapy. Functional oral intake was measured by the FOIS at baseline and at post-treatment (4 weeks). Significant between-group differences in functional oral intake were found at post-treatment, in favour of NMES sensory approach vs. NMES motor approach, in favour of NMES sensory approach vs. no NMES, and in favour of NMES motor approach vs. no NMES.
Conclusion: There is limited evidence (Level 2a) from two fair quality RCTs that NMES sensory approach + traditional swallowing therapy is more effective than comparison interventions (NMES motor approach + traditional swallowing therapy, traditional swallowing therapy alone) in improving functional oral intake among patients with acute stroke and subsequent dysphagia.
Note: Furthermore, there is limited evidence (Level 2a) from one fair quality RCT that NMES motor approach + traditional swallowing therapy is more effective than a comparison intervention (traditional swallowing therapy alone) in improving functional oral intake in patients with acute stroke and subsequent dysphagia.
Functional severity of dysphagia
Effective
1b
One high quality RCT (Huang et al., 2014) investigated the effect of neuromuscular electrical stimulation (NMES) and traditional swallowing therapy on functional severity of dysphagia in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES + traditional swallowing therapy, NMES alone, or traditional swallowing therapy alone. Functional severity of dysphagia was measured by the Functional Dysphagia Scale at baseline and post-treatment (3 weeks). Significant between-group differences in functional severity of dysphagia (solids, thick liquids) were seen at post-treatment, favoring NMES + swallowing therapy vs. NMES alone, and favoring NMES + swallowing therapy vs. traditional swallowing therapy alone. However, no significant between-group differences were found for soft diet and thin liquids.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that NMES and traditional swallowing therapy is more effective than comparison interventions (NMES alone, traditional swallowing therapy) in improving functional severity of dysphagia (solids and thick liquids only) in patients with acute stroke and subsequent dysphagia.
Note: There were no significant between-group differences on consumption of soft diet or thin liquids.
Muscle electrical activity
Effective
2a
One fair quality RCT (Xia et al., 2011) investigated the effect of neuromuscular electrical stimulation (NMES) on muscle electrical activity in patients with acute stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive NMES + traditional swallowing therapy, NMES alone or traditional swallowing therapy alone. Muscle electrical activity was measured by surface electromyography at baseline and at post-treatment (4 weeks). Significant between-group differences in muscle electrical activity were found at post-treatment, favoring NMES + traditional swallowing therapy vs. NMES alone, and favouring NMES + traditional swallowing therapy vs. traditional swallowing therapy alone.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that NMES combined with traditional swallowing therapy is more effective than comparison interventions (NMES alone, traditional swallowing therapy alone) in improving muscle electrical activity in patients with acute stroke and subsequent dysphagia.
Nutritional status
Not effective
1b
One high quality RCT (Huang et al., 2014) investigated the effect of neuromuscular electrical stimulation (NMES) and traditional swallowing therapy on nutritional status in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES + traditional swallowing therapy, NMES alone, or traditional swallowing therapy alone. Nutritional status was measured by the Functional Oral Intake Scale at baseline and post-treatment (3 weeks). No significant between-group differences in nutritional status were found at post-treatment.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that combined NMES and traditional therapy is not more effective than comparison interventions (NMES alone, traditional swallowing therapy alone) in improving nutritional status in patients with acute stroke and subsequent dysphagia.
Swallowing function
Effective
2a
Two fair quality RCTs (Xia et al., 2011, Zhang et al., 2016) investigated the effect of neuromuscular electrical stimulation (NMES) on functional swallowing in patients with acute stroke and subsequent dysphagia.
The first fair quality RCT (Xia et al., 2011) randomized patients to receive NMES + traditional swallowing therapy, NMES alone or traditional swallowing therapy alone. Swallowing function was measured by the Standardized Swallowing Assessment (SSA) at baseline and at post-treatment (4 weeks). Significant between-group differences in swallowing function were found at post-treatment, favoring NMES + traditional swallowing therapy vs. NMES alone, and favouring NMES + traditional swallowing therapy vs. traditional swallowing therapy alone.
The second fair quality RCT (Zhang et al., 2016) randomized patients to receive NMES sensory approach, NMES motor approach, or no NMES; all groups received traditional swallowing therapy. Functional swallowing was measured by the Water Swallow Test and the SSA at baseline and at post-treatment (4 weeks). Significant between group differences were found on both measures of functional swallowing at post-treatment, in favour of the NMES sensory approach vs. NMES motor approach, in favour of NMES sensory approach vs. no NMES, and in favour of NMES motor approach vs. no NMES.
Conclusion: There is limited evidence (Level 2a) from two fair quality RCTs that NMES + traditional swallowing therapy and NMES sensory approach + traditional swallowing therapy are more effective than comparison interventions (NMES alone, NMES motor approach + traditional swallowing therapy, traditional swallowing therapy alone) in improving functional swallowing among patients with acute stroke and subsequent dysphagia.
Note: Furthermore, there is limited evidence (Level 2a) from one fair quality RCT that NMES motor approach + traditional swallowing therapy is more effective in improving functional swallowing than a comparison intervention (traditional swallowing therapy alone) in patients with acute stroke and subsequent dysphagia.
Swallowing related quality of life
Effective
2a
Two fair quality RCTs (Xia et al., 2011, Zhang et al., 2016) investigated the effect of neuromuscular electrical stimulation (NMES) on swallowing related quality of life in patients with acute stroke and subsequent dysphagia.
The first fair quality RCT (Xia et al., 2011) randomized patients to receive NMES + traditional swallowing therapy, NMES alone, or traditional swallowing therapy alone. Swallowing-related quality of life was measured by the Swallowing-Related Quality of Life Scale (SWAL-QOL) at baseline and at post-treatment (4 weeks). Significant between-group differences in swallowing-related quality of life were found at post-treatment, favoring NMES + traditional swallowing therapy vs. NMES alone, and favouring NMES + traditional swallowing therapy vs. traditional swallowing therapy alone.
The second fair quality RCT (Zhang et al., 2016) randomized patients to receive NMES sensory approach, NMES motor approach, or no NMES; all groups received traditional swallowing therapy. Swallowing-related quality of life was measured by the SWAL-QOL at baseline and at post-treatment (4 weeks). Significant between-group differences in swallowing-related quality of life were found at post-treatment, in favour of NMES sensory approach vs. NMES motor approach, in favour of NMES sensory approach vs. no NMES, and in favour of NMES motor approach vs. no NMES.
Conclusion: There is limited evidence (Level 2a) from two fair quality RCTs that NMES + traditional swallowing therapy and NMES sensory approach + traditional swallowing therapy are more effective in improving swallowing-related quality of life than comparison intervention (NMES alone, NMES motor approach+ traditional swallowing therapy, traditional swallowing therapy alone) in patients with acute stroke and subsequent dysphagia.
Note: Furthermore, there is limited evidence (Level 2a) from one fair quality RCT that NMES motor approach + traditional swallowing therapy is more effective than a comparison intervention (traditional swallowing therapy alone) in improving swallowing-related quality of life among patients with acute stroke and subsequent dysphagia.
Acute phase - Pharyngeal electrical stimulation
Airway protection
Effective
1b
One high quality RCT (Jayasekeran et al., 2010) investigated the effect of pharyngeal electrical stimulation on airway protection in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation or sham pharyngeal electrical stimulation for 3 consecutive days. Airway protection was measured by the Penetration-Aspiration Scale using the videofluoroscopic examination at baseline and at 2 weeks from the beginning of the treatment. Significant between-group differences in airways protection were found at 2 weeks, favoring pharyngeal electrical stimulation vs. sham stimulation.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that pharyngeal electrical stimulation is more effective than sham stimulation in improving airway protection in patients with acute stroke and subsequent dysphagia.
Functional independence
Not effective
1b
One high quality RCT (Jayasekeran et al., 2010) investigated the effect of pharyngeal electrical stimulation on functional independence in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation or sham pharyngeal electrical stimulation for 3 consecutive days. Functional independence was measured by the Barthel Index at baseline and at discharge from the hospital. No significant between-group differences in functional independence were found at discharge.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that pharyngeal electrical stimulation is not more effective than sham stimulation in improving functional independence in patients with acute stroke and subsequent dysphagia.
Functional severity of dysphagia
Effective
1b
One high quality RCT (Jayasekeran et al., 2010) investigated the effect of pharyngeal electrical stimulation on functional severity of dysphagia in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation or sham pharyngeal electrical stimulation for 3 consecutive days. Functional severity of dysphagia was measured by the Dysphagia Severity Rating Scale at baseline and at 2 weeks from the beginning of the treatment. Significant between-group differences in functional severity of dysphagia were found at 2 weeks, favoring pharyngeal electrical stimulation vs. sham stimulation.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that pharyngeal electrical stimulation is more effective than sham stimulation in improving functional severity of dysphagia in patients with acute stroke and subsequent dysphagia.
Length of hospitalization
Effective
1b
One high quality RCT (Jayasekeran et al., 2010) investigated the effect of pharyngeal electrical stimulation on length of hospitalization in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation or sham pharyngeal electrical stimulation for 3 consecutive days. Length of hospitalization was measured at discharge from hospital. Significant between-group differences in length of hospitalization were found, favoring pharyngeal electrical stimulation vs. sham stimulation.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that pharyngeal electrical stimulation is more effective than sham stimulation in reducing length of hospitalization in patients with acute stroke and subsequent dysphagia.
Temporal swallowing measures
Not effective
1b
One high quality RCT (Jayasekeran et al., 2010) investigated the effect of pharyngeal electrical stimulation on temporal swallowing measures in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation or sham pharyngeal electrical stimulation for 3 consecutive days. Temporal swallowing measures were measured by videofluoroscopic examination at baseline and at 2 weeks from the beginning of the treatment. No significant between-group differences in temporal swallowing measures were found at 2 weeks.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that pharyngeal electrical stimulation is not more effective than sham stimulation in improving temporal swallowing measures in patients with acute stroke and subsequent dysphagia.
Acute phase - Swallowing therapy
Death or institutionalization
Effective
1b
One high quality RCT (Carnaby et al., 2006) investigated the effect of swallowing therapy on incidence of death or institutionalization in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low intensity swallowing therapy (swallowing compensatory strategies, environmental modification, safe swallowing advice, dietary modifications, 3 times per week), high intensity swallowing therapy (direct swallowing exercise, dietary modifications, 5 times per week) or usual care (patient management by the attending physician for 1 month or for the duration of hospitalization). Results from the low intensity and high intensity groups were combined due to minimal differences between the groups. Incidence of death or institutionalization was measured at 6-month follow-up. Significant between-group differences in incidence of death or institutionalization were found favoring swallowing therapy vs. usual care.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that swallowing therapy is more effective than a comparison intervention (usual care) in reducing the incidence of death or institutionalization in patients with acute stroke and subsequent dysphagia.
Functional independence
Not effective
1b
One high quality RCT (Carnaby et al., 2006) investigated the effect of swallowing therapy on functional independence in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low intensity swallowing therapy (swallowing compensatory strategies, environmental modification, safe swallowing advice, dietary modifications, 3 times per week), high intensity swallowing therapy (direct swallowing exercise, dietary modifications, 5 times per week) or usual care (patient management by the attending physician for 1 month or for the duration of hospitalization). Results from the low intensity and high intensity groups were combined due to minimal differences between the groups. Functional independence was measured by the Barthel Index and Modified Rankin Scale at baseline and at 6-month (follow-up). No significant between-group differences in functional independence were seen at 6 months.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that swallowing therapy is not more effective than a comparison intervention (usual care) in improving functional independence in patients with acute stroke and subsequent dysphagia.
Functional swallowing
Effective
1b
One high quality RCT (Carnaby et al., 2006) investigated the effect of swallowing therapy on functional swallowing in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low intensity swallowing therapy (swallowing compensatory strategies, environmental modification, safe swallowing advice, dietary modifications, 3 times per week), high intensity swallowing therapy (direct swallowing exercise, dietary modifications, 5 times per week) or usual care (patient management by the attending physician for 1 month or for the duration of hospitalization). Results from the low intensity and high intensity groups were combined due to minimal differences between the groups. Functional swallowing (i.e. return to pre-stroke diet without swallowing complications) was measured at 6-month follow-up. At 6 months there were significant between-group differences in functional swallowing, favoring swallowing therapy vs. usual care.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that swallowing therapy is more effective than a comparison intervention (usual care) in improving functional swallowing in patients with acute stroke and subsequent dysphagia.
Medical complications and aspiration pneumonia
Effective
1b
One high quality RCT (Carnaby et al., 2006) investigated the effect of swallowing therapy on swallowing-related medical complications including aspiration pneumonia in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low intensity swallowing therapy (swallowing compensatory strategies, environmental modification, safe swallowing advice, dietary modifications, 3 times per week), high intensity swallowing therapy (direct swallowing exercise, dietary modifications, 5 times per week) or usual care (patient management by the attending physician for 1 month or for the duration of hospitalization). Results from the low intensity and high intensity groups were combined due to minimal differences between the groups. Incidence of swallowing-related medical complications and aspiration pneumonia was measured at 6-month follow-up. Significant between-group differences in the incidence of swallowing-related medical complications and aspiration pneumonia were found at 6 months, favoring swallowing therapy vs. usual care.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that swallowing therapy is more effective than a comparison intervention (usual care) in reducing the incidence of swallowing-related medical complications and aspiration in patients with acute stroke and subsequent dysphagia.
Return to normal diet
Not effective
1b
One high quality RCT (Carnaby et al., 2006) investigated the effect of swallowing therapy on return to normal diet in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive low intensity swallowing therapy (swallowing compensatory strategies, environmental modification, safe swallowing advice, dietary modifications, 3 times per week), high intensity swallowing therapy (direct swallowing exercise, dietary modifications, 5 times per week) or usual care (patient management by the attending physician for 1 month or for the duration of hospitalization). Results from the low intensity and high intensity groups were combined due to minimal differences between the groups. Return to normal diet was measured at 6-month follow-up. A significant between-group difference in the number of people who had returned to their normal (pre-stroke) diet was seen at 6 months, favoring usual care vs. swallowing therapy.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that swallowing therapy is not more effective than a comparison intervention (usual care) in improving return to normal diet in patients with acute stroke and subsequent dysphagia. In fact, patients who received standard care were more likely to return to their typical diet by 6 months post-stroke than patients who received swallowing therapy.
Acute phase - Transcranial direct current stimulation (tDSC)
Functional severity of dysphagia
Effective
1a
Two high quality RCTs (Kumar et al., 2011, Joo Yang et al., 2012) investigated the effect of transcranial direct current stimulation (tDCS) on functional severity of dysphagia in patients with acute stroke and subsequent dysphagia.
The first high quality RCT (Kumar et al., 2011) randomized patients to receive anodal tDCS or sham tDCS to the sensorimotor cortical representation of swallowing in the unaffected hemisphere with standardized swallowing maneuvers. Functional severity of dysphagia was measured by the Dysphagia Outcome and Severity Scale at baseline and at post-treatment (5 days). Significant between-group differences in severity of dysphagia were found at post-treatment, favoring anodal tDCS vs sham tDCS.
The second high quality RCT (Joo Yang et al., 2011) randomized patients to receive anodal tDCS or sham tDCS to the pharyngeal motor cortex of the affected hemisphere during conventional swallowing training. Functional severity of dysphagia was measured by the Functional Dysphagia Scale at baseline, post-treatment (2 weeks) and at 3-month follow-up. While no significant between-group differences in functional severity of dysphagia were seen at post-treatment, significant differences were found at 3-month follow-up, favoring anodal tDCS vs. sham tDCS.
Conclusion: There is strong evidence (Level 1a) from two high-quality RCTs that tDCS during conventional swallowing training is more effective than sham tDCS in improving functional severity of dysphagia in patients with acute stroke and subsequent dysphagia.
Note: One of the high quality RCTs saw a significant difference in favour of anodal tDCS vs. sham tDCS at 3-month follow-up only.
Swallowing timing
Not effective
1b
One high quality RCT (Joo Yang et al., 2012) investigated the effect of transcranial direct current stimulation (tDCS) on swallowing timing in patients with acute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive anodal tDCS or sham tDCS to the pharyngeal motor cortex of the affected hemisphere during conventional swallowing training. Swallowing timing (oral transit time, pharyngeal transit time and total transit time) was measured by Videofluoroscopic Swallowing Study (VFSS) at baseline, post-treatment (2 weeks) and at 3-month follow-up. No significant between-group differences in swallowing timing were found at any time point.
Conclusion: There is moderate evidence (Level 1b) from one high-quality RCT that tDCS during conventional swallowing training is not more effective than sham tDCS in improving swallowing timing in patients with acute stroke and subsequent dysphagia.
Subacute phase - Dysphagia therapist
Aspiration pneumonia
Not effective
1b
One high quality RCT (DePippo et al., 1994) investigated the effects of dysphagia therapist-led intervention on aspiration pneumonia in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive: (a) minimal input from a dysphagia therapist (diet and swallowing exercises managed by self or a family member); (b) moderate input from a dysphagia therapist (therapist-managed diet, self-managed swallowing exercises); or (c) intensive input from a dysphagia therapist (therapist-managed diet and swallowing exercises). Incidence of aspiration pneumonia was measured at post-treatment (end point during the inpatient stay) and at follow-up (1 year post-stroke). No significant between-group differences in occurrence of aspiration pneumonia were found at either time point. However, there was a significant difference in time to pneumonia onset, whereby patients who received moderate input from the dysphagia therapist developed pneumonia sooner than patients who received minimal input.
Note: This study did not monitor frequency of dysphagia therapist intervention in group C.
Conclusion: There is moderate evidence (level 1b) from one high quality RCT that amount of input from a dysphagia therapist does not alter incidence of aspiration pneumonia among patients with subacute stroke and dysphagia.
Note: However, patients who received moderate input from the dysphagia therapist developed pneumonia sooner than patients who received minimal input.
Dehydration
Not effective
1b
One high quality RCT (DePippo et al., 1994) investigated the effect of dysphagia therapist-led intervention on dehydration in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive: (a) minimal input from a dysphagia therapist (diet and swallowing exercises managed by self or a family member); (b) moderate input from a dysphagia therapist (therapist-managed diet, self-managed swallowing exercises); or (c) intensive input from a dysphagia therapist (therapist-managed diet and swallowing exercises). Incidence of dehydration was measured at post-treatment (end point during the inpatient stay) and at follow-up (1 year post-stroke). No significant between-group differences in occurrence of dehydration were found at either time point.
Note: This study did not monitor for frequency of dysphagia therapist intervention in group C.
Conclusion: There is moderate evidence (level 1b) one high quality RCT that amount of input from a dysphagia therapist does not alter incidence of dehydration among patients with subacute stroke and dysphagia.
Malnutrition
Not effective
1b
One high quality RCT (DePippo et al., 1994) investigated the effect of dysphagia therapist-led intervention on malnutrition in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive: (a) minimal input from a dysphagia therapist (diet and swallowing exercises managed by self or a family member); (b) moderate input from a dysphagia therapist (therapist-managed diet, self-managed swallowing exercises); or (c) intensive input from a dysphagia therapist (therapist-managed diet and swallowing exercises). Malnutrition was measured by time until calorie – nitrogen deficit at baseline, post-treatment (end point during the inpatient stay) and at follow-up (1 year post-stroke). No significant between-group differences in malnutrition were found at any time point.
Note: This study did not monitor for frequency of dysphagia therapist intervention in group C.
Conclusion: There is moderate evidence (level 1b) from one high quality RCT that amount of input from a dysphagia therapist does not alter incidence of malnutrition among patients with subacute stroke and dysphagia.
Subacute phase - NMES
Bolus viscosity tolerance
Effective
1b
One high quality RCT (Terre & Mearin, 2015) investigated the effect of NMES on bolus viscosity at which aspiration occurred in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES or sham NMES; both groups received conventional swallowing therapy. Bolus viscosity at which aspiration occurred was measured by videofluorscopic examination at baseline, post-treatment (1 month) and follow-up (3 months). Significant between-group differences for bolus viscosity at which aspiration occurred were found at post-treatment, favoring NMES vs. sham NMES. These differences did not remain significant at follow-up.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that NMES is more effective, in short-term, than sham NMES in improving bolus viscosity at which aspiration occurs in patients with subacute stroke and subsequent dysphagia.
Esophageal strength and coordination
Not effective
1b
One high quality RCT (Terre & Mearin, 2015) investigated the effect of NMES on esophageal strength and coordination in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES or sham NMES; both groups received conventional swallowing therapy. Esophageal strength and coordination were measured by esophageal manometry method (basal pressure, relaxation, pharyngeal contraction) at baseline, post-treatment (1 month) and follow-up (3 months). There were no significant between-group differences in esophageal strength and coordination at any time point.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that NMES is not more effective than sham NMES in improving esophageal strength and coordination in patients with subacute stroke and subsequent dysphagia.
Functional oral intake
Effective
1b
One high quality RCT (Terre & Mearin, 2015) investigated the effect of NMES on functional oral intake in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES or sham NMES; both groups also received conventional swallowing therapy. Functional oral intake was measured by the Functional Oral Intake Scale at baseline, post-treatment (1 month) and follow-up (3 months). Significant between-group differences in functional oral intake were seen from baseline to post-treatment, favoring NMES vs. sham NMES; these improvements did not remain significant at 3-month follow-up.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that NMES is more effective, in short-term, than sham NMES in improving functional oral intake in patients with subacute stroke and subsequent dysphagia.
Satisfaction with treatment
Effective
1b
One high quality RCT (Terre & Mearin, 2015) investigated the effects of NMES on satisfaction with treatment in patients with subacute stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES and conventional swallowing therapy or sham NMES and conventional swallowing therapy. Satisfaction with treatment was measured by a 7-Point Likert Scale at post-treatment (1 month) and follow-up (3 months). Significant between-group differences were found for satisfaction with treatment at post-treatment, favoring the NMES vs. sham NMES. These significant differences were not maintained at follow-up.
Conclusion: There is moderate (Level 1b) evidence from one high quality RCT that NMES is more effective, in short-term, than sham NMES in improving satisfaction with treatment in patients with subacute stroke and subsequent dysphagia.
Chronic phase - Functional magnetic stimulation
Swallowing performance over time
Effective
1b
One high quality RCT (Momosaki et al., 2013) investigated the effect of functional magnetic stimulation (FMS) on swallowing performance over time in patients with chronic stroke and subsequent dysphagia. This high quality RCT randomized patients to receive real FMS or sham FMS over the suprahyoid muscle group. Swallowing performance over time was measured by the Timed Water-Swallow Test (inter-swallow interval, speed, capacity) at baseline and post-treatment (1 x 10-minute session). Significant between-group differences were found for swallowing speed and capacity at post-treatment, favoring real FMS vs. sham FMS.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that real FMS is more effective than sham FMS in improving swallowing speed and capacity in patients with chronic stroke and subsequent dysphagia.
Chronic phase - NMES
Biomechanical swallowing parameters
Not effective
2a
One fair quality RCT (Bulow et al., 2008) investigated the effect of neuromuscular electrical stimulation (NMES) on biomechanical swallowing parameters in patients with chronic stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive NMES or traditional swallowing therapy. Biomechanical swallowing parameters were measured by videofluoroscopic examination at baseline and post-treatment (3 weeks). No significant between-group differences were found in biomechanical swallowing parameters at post-treatment.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that NMES is not more effective than a comparison intervention (traditional swallowing therapy) in improving biomechanical swallowing parameters in patients with chronic stroke and subsequent dysphagia.
Functional nutrition
Not effective
2a
One fair quality RCT (Bulow et al., 2008) investigated the effects of NMES on functional nutrition in patients with chronic stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive NMES or traditional swallowing therapy. Functional nutrition was measured by the Actual Nutrition Scale at baseline and post-treatment (3 weeks). No significant between-group differences were found for functional nutrition at post-treatment.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that NMES is not more effective than a comparison intervention (traditional swallowing therapy) in improving functional nutrition in patients with chronic stroke and subsequent dysphagia.
Oral motor function
Not effective
2a
One fair quality RCT (Bulow et al., 2008) investigated the effect of NMES on oral motor function in patients with chronic stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive NMES or traditional swallowing therapy. Oral motor function was measured by the Oral Motor Function Scale at baseline and post-treatment (3 weeks). No significant between-group differences were found in oral motor function at post-treatment.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that NMES is not more effective than a comparison intervention (traditional swallowing therapy) in improving oral motor function in patients with chronic stroke and subsequent dysphagia.
Self-evaluation of dysphagia
Not effective
2a
One fair quality RCT (Bulow et al., 2008) investigated the effect of NMES on self-evaluation of dysphagia in patients with chronic stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive NMES or traditional swallowing therapy. Self-evaluation of dysphagia was measured using a 5-point Visual Analogue Scale at baseline and post-treatment (3 weeks). No significant between-group differences were found for self-evaluation of dysphagia at post-treatment.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that NMES is not more effective than a comparison intervention (traditional swallowing therapy) in improving self-evaluation of dysphagia in patients with chronic stroke and subsequent dysphagia.
Chronic phase - NMES & effortful swallow
Airway protection
Effective
1b
One high quality RCT (Park et al., 2016) investigated the effect of combined NMES and effortful swallow on airway protection in patients with chronic stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES to the point of effortful swallow (motor NMES) or NMES alone (sensory NMES). Airway protection was measured by the Penetration-Aspiration Scale at baseline and post-treatment (6 weeks). Significant between group differences were found for airway protection at post-treatment, favoring motor NMES vs. sensory NMES.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that motor NMES is more effective than sensory NMES in improving airway protection in patients with chronic stroke and subsequent dysphagia.
Biomechanical swallowing parameters
Effective
1b
One high quality RCT (Park et al., 2016) investigated the effect of NMES and effortful swallow on biomechanical swallowing parameters in patients with chronic stroke and subsequent dysphagia. This high quality RCT randomized patients to receive NMES to the point of effortful swallow (motor NMES) or NMES alone (sensory NMES). Biomechanical swallowing parameters were measured by the Videofluoroscopic Dysphagia Scale (VDS – total, oral phase, pharyngeal phase), and horizontal and vertical displacement of the hyoid bone on videofluoroscopic swallowing study at baseline and post-treatment (6 weeks). Significant between-group differences were found for all biomechanical swallowing parameters (except VDS – oral phase) at post-treatment, favoring motor NMES vs sensory NMES.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that motor NMES is more effective than sensory NMES in improving biomechanical swallowing parameters in patients with chronic stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - Combined central and peripheral neurostimulation
Airway protection
Effective
1b
One high quality RCT (Michou et al., 2014) investigated the effect of combined central and peripheral forms of neurostimulation on airway protection in patients with subacute or chronic stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation (PES), paired associative stimulation (PAS), repetitive transcranial magnetic stimulation (rTMS), or the respective sham treatments (i.e. sham PES, sham PAS, sham rTMS). Airway protection was measured by the Penetration-Aspiration Scale using videofluoroscopic assessment at baseline and 30 minutes post-treatment. When results of all three real modalities were combined, a significant between-group difference was found in airway protection, favoring combined central and peripheral neurostimulation vs. sham neurostimulation.
Conclusion: There is moderate (Level 1b) evidence from one high quality RCT that combined central and peripheral forms of neurostimulation is more effective than sham stimulation in improving airway protection in patients with subacute or chronic stroke and subsequent dysphagia.
Cortical excitability
Effective
1b
One high quality RCT (Michou et al., 2014) investigated the effect of combined central and peripheral forms of neurostimulation on cortical excitability in patients with subacute or chronic stroke and subsequent dysphagia. This high quality RCT randomized patients to receive pharyngeal electrical stimulation (PES), paired associative stimulation (PAS), repetitive transcranial magnetic stimulation (rTMS), or the respective sham treatments (i.e. sham PES, sham PAS, sham rTMS). Corticobulbar excitability of the pharyngeal motor cortex was measured at baseline and 30 minutes post-treatment. Significant between-group differences were found in corticobulbar excitability of the pharyngeal motor cortex of the unaffected hemisphere, favoring PES vs. sham PES and PAS vs. sham PAS. No significant between-treatment differences were found in corticobulbar excitability of the pharyngeal motor cortex of the unaffected hemisphere for rTMS vs. sham rTMS. Moreover, when results of all three real modalities were combined, a significant between-treatment difference was found in the corticobulbar excitability of the pharyngeal motor cortex of the unaffected hemisphere, favoring combined central and peripheral neurostimulation vs. sham neurostimulation.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that combined central and peripheral forms of neurostimulation is more effective than sham stimulation in improving corticobulbar excitability of the pharyngeal motor cortex of the unaffected hemisphere in patients with subacute or chronic stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - Mendelsohn maneuver
Airway protection
Not effective
2a
One fair quality RCT (McCullough & Kim, 2013; results also reported in McCullough et al., 2012) investigated the effect of the Mendelsohn maneuver on airway protection in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive the Mendelsohn maneuver or no treatment. Airway protection was measured by the Penetration-Aspiration Scale (PAS) at baseline, post-treatment (2 weeks) and at 3-month follow-up. No significant between-group differences in airway protection were found at either time point.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that the Mendelsohn maneuver is not more effective than no treatment in improving airway protection in patients with stroke and subsequent dysphagia.
Biomechanical swallowing parameters
Not effective
2a
One fair quality RCT (McCullough & Kim, 2013) investigated the effect of Mendelsohn maneuver on biomechanical swallowing parameters in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive the Mendelsohn maneuver or no treatment. Biomechanical swallowing parameters were measured by Videofluoroscopic Swallowing Study (VFSS – hyoid maximum elevation, hyoid maximum anterior excursion, extent of upper esophageal sphincter opening) at baseline, post-treatment (2 weeks) and at 3-month follow-up. There were no significant between-group differences in any biomechanical swallowing parameter at any time point.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that the Mendelsohn maneuver is not more effective than no treatment in improving biomechanical swallowing parameters in patients with stroke and subsequent dysphagia.
Functional severity of dysphagia
Not effective
2a
One fair quality RCT (McCullough & Kim, 2013; results also reported in McCullough et al., 2012) investigated the effect of the Mendelsohn maneuver on functional severity of dysphagia in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive the Mendelsohn maneuver or no treatment. Functional severity of dysphagia was measured by the Dysphagia Outcome and Severity Scale (DOSS) at baseline, post-treatment (2 weeks) and at 3-month follow-up. No significant between-group differences in functional severity of dysphagia were found at any time point.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that the Mendelsohn maneuver is not more effective than no treatment in improving functional severity of dysphagia in patients with stroke and subsequent dysphagia.
Swallowing timing
Not effective
2a
One fair quality RCT (McCullough et al., 2012) investigated the effect of the Mendelsohn maneuver on swallowing timing in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive the Mendelsohn maneuver or no treatment. Swallowing timing was measured by Videofluoroscopic Swallowing Study (VFSS – duration of: hyoid maximum anterior excursion, hyoid maximum elevation, pharyngeal response, upper esophageal sphincter opening) at baseline and post-treatment (2 weeks). No significant between-group differences in swallowing timing were found at post-treatment.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that the Mendelsohn maneuver is not more effective than no treatment in improving swallowing timing in patients with stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - Motor electrical stimulation & effortful swallow
Airway protection
Insufficient evidence
5
One fair quality RCT (Park et al., 2012) investigated the effect of combined effortful swallow with infrahyoid motor electrical stimulation on airway protection in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive either infrahyoid motor electrical stimulation or infrahyoid sensory electrical stimulation. Airway protection was measured by the Penetration-Aspiration Scale (PAS) on effortful swallow at baseline and at post-treatment (4 weeks). Between-group differences in airway protection were not reported; there were no significant within-group differences in airway protection from baseline to post-treatment in either group.
Conclusion: There is insufficient evidence (Level 5) regarding the effect of motor electrical stimulation on airway protection. A fair quality RCT found no significant change in airway protection following motor or sensory electrical stimulation.
Biomechanical swallowing parameters
Insufficient evidence
5
One fair quality RCT (Park et al., 2012) investigated the effect of combined effortful swallow with infrahyoid motor electrical stimulation on biomechanical swallowing parameters in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive either infrahyoid motor electrical stimulation or infrahyoid sensory electrical stimulation. Biomechanical swallowing parameters were measured on effortful swallow by the Videofluoroscopic Swallowing Study (VFSS) at baseline and at post-treatment (4 weeks). Between-group differences in biomechanical swallowing parameters were not reported. Within-group comparison revealed a significant increase in vertical movement of the larynx from baseline to post-treatment in the motor electrical stimulation group, whereas the sensory electrical stimulation group showed no significant differences in biomechanical swallowing parameters from baseline to post-treatment.
Conclusion: There is insufficient evidence (Level 5) regarding the effect of motor electrical stimulation on biomechanical swallowing parameters. However, a fair quality RCT found a significant increase in the vertical movement of the larynx from baseline to post-treatment in the motor electrical stimulation group but not the sensory electrical stimulation group.
Phase of stroke recovery not specific to one period - NMES & physical therapy
Biomechanical swallowing parameters
Effective
2a
One fair quality RCT (El-Tamawy et al., 2015) investigated the effect of physical therapy and neuromuscular electrical stimulation (NMES) on biomechanical swallowing parameters in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive physical therapy+NMES or medical care alone. Physical therapy was directed at strengthening and stimulating the elevator muscles of the larynx above and below the hyoid bone. Biomechanical swallowing parameters were measured by VideoFluoroscopic Swallowing Study (VFSS – oral transit time, hyoid elevation, laryngeal elevation, esophageal sphincter opening, aspiration/penetration) at baseline and post-treatment (6 weeks). Significant between group differences in all biomechanical swallowing parameters except oesophageal sphincter opening were found at post-treatment, favoring physical therapy+NMES vs. medical care alone.
Conclusion: There is limited (Level 2a) evidence that physical therapy + NMES is more effective than a comparison intervention (medical care alone) in improving biomechanical swallowing parameters in patients with stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - NMES & tactile-thermal stimulation
Airway protection
Effective
1b
One high quality RCT (Lim et al., 2009) investigated the effect of combined neuromuscular electrical stimulation (NMES) and thermal-tactile stimulation (TTS) on airway protection in patients stroke and subsequent dysphagia. This high quality RCT randomized patients to receive combined NMES+TTS or TTS alone. Airway protection during consumption of semi-solids and liquids was measured by the Rosenbek Penetration-Aspiration Scale at baseline and at post-treatment (4 weeks). Significant between-group differences in airway protection (semi-solids and liquids) were found at post-treatment, favoring NMES+TSS vs. TSS alone.
Conclusion: There is moderate evidence (level 1b) from 1 high quality RCT that combined neuromuscular electrical stimulation and tactile-thermal stimulation is more effective than tactile-thermal stimulation alone in improving airway protection in patients with stroke and subsequent dysphagia.
Swallowing function
Effective
1b
One high quality RCT (Lim et al., 2009) investigated the effect of combined neuromuscular electrical stimulation (NMES) and thermal-tactile stimulation (TTS) on swallowing function in patients with stroke and subsequent dysphagia. This high quality RCT randomized patients to receive combined NMES+TTS or TTS alone. Swallowing function was measured by the Swallow Function Scoring system at baseline and post-treatment (4 weeks). Significant between-group differences in swallowing function were found at post-treatment, favoring combined NMES+TSS vs. TSS alone.
Conclusion: There is moderate evidence (Level 1b) from 1 high quality RCT that combined neuromuscular electrical stimulation and tactile-thermal stimulation is more effective than tactile-thermal stimulation alone in improving swallowing function in patients with stroke and subsequent dysphagia.
Swallowing timing
Effective
1b
One high quality RCT (Lim et al., 2009) investigated the effect of combined neuromuscular electrical stimulation (NMES) and thermal-tactile stimulation (TTS) on swallowing timing in patients with stroke and subsequent dysphagia. This high quality RCT randomized patients to receive combined NMES+TTS or TTS alone. Pharyngeal transit timing on consumption of semi-solids and liquids was measured by videofluoroscopic imaging at baseline and post-treatment (4 weeks). Significant between-group differences were found for swallow timing at post-treatment, favoring NMES+TSS vs. TSS alone.
Conclusion: There is moderate evidence (Level 1b) from 1 high quality RCT that combined neuromuscular electrical stimulation and tactile-thermal stimulation is more effective than tactile-thermal stimulation alone in improving swallow timing in patients with stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - Olfactory stimulation
Cough-reflex sensitivity
Not effective
2a
One fair quality RCT (Ebihara et al., 2006) investigated the effect of olfactory stimulation on cough reflex sensitivity in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive black pepper oil stimulation, lavender oil stimulation, or nasal inhalation of distilled water. Cough reflex sensitivity was measured at baseline and post-treatment (30 days). No significant between-group differences in cough reflex sensitivity were found at post-treatment.
Conclusion: There is limited evidence (Level 2a) from 1 fair quality RCT that olfactory stimulation using black pepper oil is not more effective than comparison interventions (lavender oil stimulation, nasal inhalation of distilled water) in improving cough-reflex sensitivity in patients with stroke and subsequent dysphagia.
Number of swallowing movements
Effective
2a
One fair quality RCT (Ebihara et al., 2006) investigated the effect of olfactory stimulation on the number of swallowing movements in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive olfactory stimulation using black pepper oil, lavender oil, or distilled water. The number of swallowing movements was measured at baseline and post-treatment (30 days). Significant between-group differences in the number of swallowing movements were found at post-treatment, favoring black pepper oil vs. lavender oil and favoring black pepper oil vs. distilled water.
Conclusion: There is limited evidence (Level 2a) from 1 fair quality RCT that olfactory stimulation using black pepper oil is more effective than comparison interventions (lavender oil, distilled water) in increasing the number of swallowing movements in patients with stroke and subsequent dysphagia.
Risk of aspiration
Effective
2a
One fair quality RCT (Ebihara et al., 2006) investigated the effect of olfactory stimulation on risk of aspiration in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive olfactory stimulation using black pepper oil, lavender oil or distilled water. Risk of aspiration was measured according to Serum Substance P release, at baseline and post-treatment (30 days). Significant between-group differences in Serum Substance P levels were found at post-treatment, favoring black pepper oil vs. lavender oil and favoring black pepper oil vs. distilled water, indicating reduced risk of aspiration following this treatment.
Conclusion: There is limited evidence (Level 2a) from 1 fair quality RCT that olfactory stimulation using black pepper oil is more effective than comparison interventions (lavender oil, distilled water) in reducing risk of aspiration in patients with stroke and subsequent dysphagia.
Swallowing reflex
Effective
2a
One fair quality RCT (Ebihara et al., 2006) investigated the effect of olfactory stimulation on swallowing reflex latency in patients with stroke and subsequent dysphagia. This fair quality RCT randomized patients to receive olfactory stimulation using black pepper oil, lavender oil, or distilled water. Swallowing reflex latency was measured by the Swallowing Reflex Timed test at baseline and post-treatment (30 days). Significant between-group differences in latency of swallowing reflex were found at post-treatment, favoring black pepper oil vs. lavender oil, and favoring black pepper oil vs. distilled water.
Conclusion: There is limited evidence (Level 2a) from 1 fair quality RCT that olfactory stimulation using black pepper oil is more effective than comparison interventions (lavender oil, distilled water) in improving latency of swallowing reflex in patients with stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - Repetitive transcranial magnetic stimulation (rTMS)
Airway protection
Insufficient evidence
5
One high quality RCT (Park et al., 2013) investigated the effect of repetitive transcranial stimulation (rTMS) on airway protection in patients with stroke and subsequent dysphagia. This high quality RCT randomized patients to receive either active rTMS t or sham rTMS to the contralesional pharyngeal motor cortex. Airway protection was measured by the Penetration-Aspiration Scale (PAS) at baseline, post-treatment (2 weeks) and at 4-week follow-up. Between-group differences in airway protection were not reported; neither group demonstrated a significant change in airway protection from baseline to post-treatment and from baseline to follow-up.
Conclusion: There is insufficient evidence (Level 5) regarding the effectiveness of rTMS vs. sham rTMS in improving airway protection in patients with stroke. One high quality RCT reported no significant change in airway protection following rTMS or sham rTMS.
Degree of dysphagia
Effective
1b
Two high quality RCTs (Khedr & Abo-Elfetoh, 2010, Park et al., 2013) investigated the effect of repetitive transcranial stimulation (rTMS) on degree of dysphagia in patients with stroke and subsequent dysphagia.
The first high quality RCT (Khedr & Abo-Elfetoh, 2010) randomized patients to receive either active rTMS or sham rTMS over the oesophageal motor cortex. Degree of dysphagia was measured by a 4-point non-standardized grading scale at baseline, post-treatment (5 days), and at 1-month and 2-month follow-up. Significant between-group differences in degree of dysphagia were found at all time points, favoring active rTMS vs. sham rTMS.
The second high quality RCT (Park et al., 2013) randomized patients to receive either active rTMS or sham rTMS to the contralesional pharyngeal motor cortex. Degree of dysphagia was measured by the Videofluoroscopic Dysphagia Scale (VDS) at baseline, post-treatment (2 weeks) and 4-week follow-up. Between-group differences were not reported. However, within-group analysis showed significant improvement in degree of dysphagia from baseline to post-treatment and from baseline to follow-up in the active rTMS group only.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that that active rTMS is more effective than sham rTMS in improving degree of dysphagia in patients with stroke. Furthermore, a high quality RCT also reported a significant improvement in degree of dysphagia following rTMS.
Functional independence
Effective
1b
One high quality RCT (Khedr & Abo-Elfetoh, 2010) investigated the effect of repetitive transcranial stimulation (rTMS) on functional independence in patients with stroke and subsequent dysphagia. This high quality RCT randomized patients to receive active rTMS or sham rTMS over the oesophageal motor cortex. Functional independence was measured by the Barthel Index at baseline, post-treatment (5 days) and at 1-month and 2-month follow-up. Significant between-group differences in functional independence were seen at all time points among patients with lateral medullary infarction (but not other brainstem infarctions), favoring active rTMS vs. sham rTMS.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that active rTMS is more effective than sham rTMS in improving functional independence in patients with stroke (specifically lateral medullary infarction but not brainstem infarction) and subsequent dysphagia.
Neurological recovery
Not effective
1b
One high quality RCT (Khedr & Abo-Elfetoh, 2010) investigated the effect of repetitive transcranial stimulation (rTMS) on neurological recovery of patients with stroke and subsequent dysphagia. This high quality RCT randomized patients to receive either active rTMS or sham rTMS over the oesophageal motor cortex. Neurological recovery was measured by the National Institutes of Health Stroke Scale (NIHSS) and the Hemispheric Stroke Scale at baseline, post-treatment (5 days) and at 1-month and 2-month follow-up. No significant between-group differences in recovery were seen at any time point.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that active rTMS is not more effective than sham rTMS in improving neurological recovery of patients with stroke and subsequent dysphagia.
Phase of stroke recovery not specific to one period - tDCS
Functional severity of dysphagia
Effective
1b
One high quality RCT (Shigematsy et al., 2013) investigated the effect of transcranial direct stimulation (tDCS) with on functional severity of dysphagia in patients with stroke and subsequent dysphagia. This high quality RCT randomized patients to receive anodal tDCS or sham tDCS to the ipsilesional pharyngeal motor cortex; both groups received simultaneous conventional swallowing therapy. Functional severity of dysphagia was measured by the Dysphagia Outcome and Severity Scale (DOSS) at baseline, post-treatment (10 days) and at 1-month follow-up. Significant between-group differences in functional severity of dysphagia were found at post-treatment and at follow-up, favoring anodal tDCS vs. sham tDCS.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that anodal tDCS is more effective than sham tDCS in improving functional severity of dysphagia in patients with stroke and subsequent dysphagia.
References
Bulow, M., Speyer, R., Baijens, L., Woisard, V., & Ekberg, O. (2008). Neuromuscular electrical stimulation (NMES) in stroke patients with oral and pharyngeal dysphagia. Dysphagia, 23, 302-9.
http://www-ncbi-nlm-nih-gov.proxy3.library.mcgill.ca/pubmed/18437464
Carnaby G, Hankey GJ, Pizzi J. (2006). Behavioural intervention for dysphagia in acute stroke: A randomised controlled trial. Lancet Neurology, 5, 31-7.
http://www.ncbi.nlm.nih.gov/pubmed/16361020
Chipps, E., Gatens, C., Genter, L., Musto, M., Dubis-Bohn, A., Gliemmo, M., Dudley, K., Holloman, C., Hoet, A.E., & Landers, T. (2014). Pilot study of an oral care protocol on poststroke survivors. Rehabilitation Nursing. 39(6), 294-304.
https://www.ncbi.nlm.nih.gov/pubmed/25131413
DePippo K.L., Holas M.A., Reding M.J., Mandel F.S., Lesser M.L. (1994). Dysphagia therapy following stroke: A controlled trial. Neurology, 44, 1655-1660.
http://www.ncbi.nlm.nih.gov/pubmed/7936292
Ebihara T., Ebihara S., Maruyama M., Kobayashi M., Itou A., Arai H., Sasaki H. (2006). A randomized trial of olfactory stimulation using black pepper oil in older people with swallowing dysfunction. Journal of the American Geriatrics Society. 54, 1401-6.
http://www.ncbi.nlm.nih.gov/pubmed/16970649
El-Tamawy, M., Darwish, M.H., El-Azizi, H.S., Abdelalim, A.M., & Taha, S.I. (2015). The influence of physical therapy on oropharyngeal dysphagia in acute stroke patients. Egyptian Journal of Neurology Psychiatry and Neurosurgery, 52, 201-205.
https://www.researchgate.net/publication/281537852_The_influence_of_physical_therapy_on_oropharyngeal_dysphagia_in_acute_stroke_patients
Huang, K-L., Liu, T-Y., Huang, Y-C., Leong, C-P., Lin, W-C., & Pong, Y-P. (2014). Functional outcome in acute patients with oropharyngeal dysphagia after swallowing therapy. Journal of Stroke and Cerebrovascular Diseases, 23(10), 2547-53.
http://www.ncbi.nlm.nih.gov/pubmed/25245482
Jayasekeran, V., Singh, S., Tyrrell, P., Michou, E., Jefferson, S., Mistry, S., & Hamdy, S. (2010). Adjunctive functional pharyngeal electrical stimulation reverses swallowing disability after brain lesions. Gastroenterology, 138(5), 1737-1746.
http://www.sciencedirect.com/science/article/pii/S0016508510001617
Joo Yang, E.J., Baek, S-R., Shin, J., Lim, J.Y., Kim, Y.K., & Paik, N.J. (2012). Effects of transcranial direct current stimulation (tDCS) on post-stroke dysphagia. Restorative Neurology and Neuroscience, 30, 303-11.
http://www.ncbi.nlm.nih.gov/pubmed/22572022
Khedr, E. & Abo-Elfetoh, N. (2010). Therapeutic role of rTMS on recovery of dysphagia in patients with lateral medullary syndrome and brainstem infraction. Journal of Neurology Neurosurgery and Psychiatry, 81, 495-99.
http://www.ncbi.nlm.nih.gov/pubmed/19828479
Kumar, S., Wagner, C.W., Frayne, C., Zhu, L., Selim, M., Feng, W., & Schlaug, G. (2011). Noninvasive brain stimulation may improve stroke-related dysphagia: a pilot study. Stroke, 42, 1035-40.
http://www.ncbi.nlm.nih.gov/pubmed/21441148
Lim K.B., Lee H.-J.L., Lim S.-S., Choi Y.-I., (2009). Neuromuscular Electrical and Thermal-Tactile Stimulation for Dysphagia Caused by Stroke: A Randomized Controlled Trial. Journal of Rehabilitation Medicine, 41(3), 174-178.
http://www.ncbi.nlm.nih.gov/pubmed/19229451
McCullough, G.H., Kamarunas, E., Mann, G.C., Schmidley, J.W., Robbins, J.A., Crary, M.A. (2012). Effects of Mendelsohn maneuver on measures of swallowing duration post-stroke. Topics in Stroke Rehabilitation, 19(3), 234-43.
http://www.ncbi.nlm.nih.gov/pubmed/22668678
McCullough, G.H., & Kim, Y. (2013). Effects of Mendelsohn maneuver on extent of hyoid movement and UES opening post-stroke. Dysphagia, 28, 511-19.
http://www.ncbi.nlm.nih.gov/pubmed/23494471
Michou, E., Mistry, S., Jefferson, S., Tyrrell, P., & Hamdy, S. (2014). Characterizing the mechanisms of central and peripheral forms of neurostimulation in chronic dysphagic stroke patients. Brain Stimulation, 7(1), 66-73.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3893483/
Momosaki, R., Masahiro, A., Watanabe, S., Kakuda, W., Yamada, N., & Mochio, K. (2014). Functional magnetic stimulation using a parabolic coil for dysphagia after stroke. Neuromodulation, 17, 637-41.
http://www.ncbi.nlm.nih.gov/pubmed/24320695
Park, J-W., Kim, Y., Oh, J-C., & Lee, H-J. (2012). Effortful swallowing training combined with electrical stimulation in post-stroke dysphagia: a randomized controlled study. Dysphagia, 27, 521-27.
http://www.ncbi.nlm.nih.gov/pubmed/22447240
Park, J-W., Oh, J-C., Lee, J-W., Yeo, J-S., Ryu, K-H. (2013). The effects of 5Hz high-frequency rTMS over contralesional pharyngeal motor cortex in post-stroke oropharyngeal dysphagia: a randomized controlled study. Neurogastroenterology and Motility, 25(4), 324-e250.
http://www.ncbi.nlm.nih.gov/pubmed/23279198
Park, J-S., Oh, D-H., Hwang, N-K., & Lee, J-H. (2016). Effects of neuromuscular electrical stimulation combined with effortful swallowing on spot-stroke oropharyngeal dysphagia: a randomized controlled trial. Journal of Oral Rehabilitation, 43, 426-34.
http://www.ncbi.nlm.nih.gov/pubmed/26969528
Power M. L., Fraser C.H., Hobson A., Singh S., Tyrrell P., Nicholson D.A., Turnbull I., Thompson D.G. & Hamdy S. (2006). Evaluating oral stimulation as a treatment for dysphagia after stroke. The Journal of Dysphagia, 49-55.
http://www.ncbi.nlm.nih.gov/pubmed/16544087
Shigematsy, T., Fujishima, I., & Ohno, K. (2013). Transcranial direct current stimulation improves swallowing function in stroke patients. Neurorehabilitation and Neural Repair, 27(4), 363-69.
http://www.ncbi.nlm.nih.gov/pubmed/23392916
Terré, R., & Mearin, F. (2015). A randomized controlled study of neuromuscular electrical stimulation in oropharyngeal dysphagia secondary to acquired brain injury. European Journal of Neurology, 22(4), 687-e44.
http://onlinelibrary.wiley.com/doi/10.1111/ene.12631/full
Woo Lee, K.W., Kim, S.B., Lee, J.H., Lee, S.J., Ri, J.W., & Park, G.J. (2014). The effect of early neuromuscular electrical stimulation therapy in acute/subacute ischemic stroke patients with dysphagia. Annals of Rehabilitation Medicine, 38(2), 153-9.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4026600/
Xia, W., Zheng, C., Zhu, S., & Tang, Z. (2016). Does the addition of specific acupuncture to standard swallowing training improve outcomes in patients with dysphagia after stroke? A randomized controlled trial. Clinical Rehabilitation, 30(3), 237-246.
http://www.ncbi.nlm.nih.gov/pubmed/25819076
Xia, W., Zheng, C., Lei, Q., Tang, Z., Hua, Q., Zhang, Y., & Zhu, S. (2011). Treatment of post-stroke dysphagia by VitalStim therapy coupled with conventional swallowing training. Journal of Huazhong University of Science and Technology, 31(1), 73-6.
http://www.ncbi.nlm.nih.gov/pubmed/21336727
Zhang, M., Tao, T., Zhang, Z-B., Zhu, X., Fan, W-G., Pu, L-J., Chu, L., & Yue, S-W. (2016). Effectiveness of neuromuscular electrical stimulation on patients with dysphagia with medullary infraction. Archives of Physical Medicine and Rehabilitation, 97, 355-62.
http://www.ncbi.nlm.nih.gov/pubmed/26606872
Zhao, J-W., Wang, Z-Y., Cao, W-Z., Zhang, Y-W., Song, S-C., Kang, W-G., & Yang, J-H. (2015). Therapeutic efficacy of swallowing neuromuscular electrical stimulation combined with acupuncture for post-stroke dysphagia. World Journal of Acupuncture-Moxibustion, 25(1), 19-23.
http://www.sciencedirect.com/science/article/pii/S1003525715300040
Excluded Studies:
Allison, M.C., Morris, A.J., Park, R.H.R., & Mills P.R. (1992). Percutaneous endoscopic gastrostomy tube feeding may improve outcome of late rehabilitation following stroke. Journal of the Royal Society of Medicine, 85 (3), 147-149.
Reason for exclusion: Not RCT.
Carnaby-Mann, G.D. & Crary, M.A. (2008). Adjuctive neuromuscular electrical stimulation for treatment-refractory dysphagia. Annals of Otology, Rhinology & Laryngology, 117(4), 279-87.
Reason for exclusion: Quasi-experimental study design, not RCT.
Cheng, I., Chan, K., Wong, C.S., & Cheung, R. (2015). Preliminary evidence of the effects of high-frequency repetitive transcranial magnetic stimulation (rTMS) on swallowing functions in post-stroke individuals with chronic dysphagia. International Journal of Language & Communication Disorders, 50(3), 389-96.
Reason for exclusion: Case series study design, not RCT.
Crary, M.A., Carnaby, G.D., Lagorio, L.A., & Carvajal, P.J. (2012). Functional and physiological outcomes from an exercise-based dysphagia therapy: a pilot investigation of the McNeill dysphagia therapy program. Archives of Physical Medicine and Rehabilitation, 93, 1173-8.
Reason for exclusion: Quasi-experimental study design, not RCT.
Crary M.A. (1995). A direct intervention program for chronic neurogenic dysphagia secondary to brainstem stroke. Dysphagia, 10(1), 6-18.
Reason for exclusion: Not RCT.
Crary M.A., Carnaby G.D., Groher M.E., Helseth E. (2004). Functional benefits of dysphagia therapy using adjunctive sEMG biofeedback. Dysphagia, 19(3), 160-164.
Reason for exclusion: Not RCT.
Gallas, S., Marie, J.P., Leroi, A.M., & Verin, E. (2010). Sensory transcutaneous electrical stimulation improves post-stroke dysphagic patients. Dysphagia, 25, 291-7.
Reason for exclusion: Quasi-experimental study design, not RCT.
Garon B.R., Engle M., Ormiston C. (1997). A randomized control study to determine the effects of unlimited oral intake of water in patients with identified aspiration. Neurorehabilitation and Neural Repair, 11, 139-148.
Reason for exclusion: Nature of intervention is compensatory
Goulding R., Bakheit AM. (2000). Evaluation of the benefits of monitoring fluid thickness in the dietary management of dysphagic stroke patients. Clinical Rehabilitation, 14, 119-24.
Reason for exclusion: Nature of intervention is compensatory.
Finestone, H.M., Foley, N.C., Woodbury, M.G., Greene-Finestone, L. (2001). Quantifying fluid intake in dysphagic stroke patients: A preliminary comparison of oral and nonoral strategies. Archives of Physical Medicine and Rehabilitation, 82, 1744- 1746.
Reason for exclusion: Not RCT.
Hagg, M. & Larsson, B. (2004). Effects of Motor and Sensory Stimulation in Stroke Patients with Long-Lasting Dysphagia. Dysphagia, 19, 219-230.
Reason for exclusion: Not RCT.
Hagg M. & Anniko M. (2008). Lip muscle training in stroke patients with dysphagia. Acta Oto-Laryngologica, 128, 1027-1033.
Reason for exclusion: Not RCT.
Hamidon B.B., Abdullah S.A., Zawawi M. F., Sukumar N., Aminuddin A., Raymond A.A. (2006). A prospective comparison of percutaneous endoscopic gastrostomy and nasogastric tube feeding in patients with acute dysphagic stroke. The Medical journal of Malaysia, 61(1), 59 -66.
Reason for exclusion: Nature of intervention
Huang, J.Y., Zhang, D.Y., Yao, Y., Xia, Q.X., Fan, Q.Q. (2006). Training in swallowing prevents aspiration pneumonia in stroke patients with dysphagia. The Journal of International Medical Research, 34, 303-306.
Reason for exclusion: Not RCT.
Kim, S.J. (2010). Music therapy protocol development to enhance swallowing training for stroke patients with dysphagia. Journal of Music Therapy, XLVII (2), 102-19.
Reason for exclusion: Case series study design, not RCT.
Lemoncello, R., Sohlberg, M.K., Fickas, S., Albin, R., & Harn, B.E. (2010). Phase I evaluation of the television assisted prompting system to increase completion of home exercises among stroke survivors. Disability and Rehabilitation: Assistive Technology, 6(5), 440-52.
Reason for exclusion: Case-series study design, not RCT.
Lin, L. C., Wang, S. C., Chen, S. H., Wang, T. G., Chen, M. Y., & Wu, S. C. (2003). Efficacy of swallowing training for residents following stroke. Journal of advanced nursing, 44(5), 469-478.
Reason for exclusion: Not RCT.
Logemann, J.A., Rademaker, A., Pauloski, B.R., Kelly, A., Stangl-McBreen, A., Antinoja, J., Grande, B., Farquharson, J., Kern, M., Easterling, C., & Shaker, R. (2009). A randomize study comparing the Shaker exercise with traditional therapy: a preliminary study. Dysphagia, 24, 403-11.
Reason for exclusion: Other population than patients with stroke.
Nam, H. S., Beom, J., Oh, B. M., & Han, T. R. (2013). Kinematic effects of hyolaryngeal electrical stimulation therapy on hyoid excursion and laryngeal elevation. Dysphagia, 28(4), 548-556.
Reason for exclusion: Mixed sample with no indication to the percentage of those with stroke vs. brain injury.
Norton B., Homer-Ward M., Donnelly M.T., Long R.G., Holmes G.K. (1996). A randomised prospective comparison of percutaneous endoscopic gastrostomy and nasogastric tube feeding after acute dysphagic stroke. British Medical Journal, 312(7022), 13-16.
Reason for exclusion: Nature of intervention.
Park R.H.R, Allison M.C., Lang J., Spence E., Morris A.J, Danesh B.J.Z., Russell R.I., Mills P.R. (1992). Randomised comparison of percutaneous endoscopic gastrostomy and nasogastric tube feeding in patients with persisting neurological dysphagia. British Medical Journal, 304(6839), 1406-1409.
Reason for exclusion: Nature of intervention
Reddy N.P., Simcox D.L., Gupta V., Motta G.E., Coppenger J., Das A., Buch O. (2000). Biofeedback therapy using accelerometry for treating dysphagic patients with poor laryngeal elevation: Case studies. Journal of Rehabilitation Research and Development, 37(3), 361-372.
Reason for exclusion: Not RCT.
Robbins J.A., Kays S.A., Gangon R.E., Hind J.A., Hewitt A.L., Gentry L.R., Taylor A.J. (2007) The effects of lingual exercise in stroke patients with dysphagia. Archives of Physical Medicine and Rehabilitation, 88, 150-8
Reason for exclusion: Not RCT.
Rosenbek J.C., Robbins J., Willford W.O. et al. (1998) Comparing treatment intensities of tactile-thermal application. Dysphagia, 13, 1-9.
Reason for exclusion: Both groups received intervention of interest, only the intensity was varied across groups.
Rosenbek J.C., Roecker E.B., Wood J.L. et al. (1996). Thermal application reduces the duration of stage transition in dysphagia after stroke. Dysphagia, 11, 225-33.
Reason for exclusion: Both groups received intervention of interest, only the intensity was varied across groups.
Shaker R., Easterling C., Kern M., Nitschke T., Massey B., Daniels S., Grande B., Kazandjian M., & Dikeman K. (2002). Rehabilitation of swallowing by exercise in tube-fed patients with pharyngeal dysphagia secondary to abnormal UES opening. Gastroenterology, 122 (5), 1314-1321.
Reason for exclusion: Nature of intervention.
Sun, S-F., Hsu, C-W., Lin, H-S., Sun, H-P., Chang, P-H., Hsieh, W-L., & Wang, J-L. (2013). Combined neuromuscular electrical stimulation (NMES) and fiberoptic endoscopic evaluation of swallowing (FEES) and traditional swallowing rehabilitation in the treatment of stroke-related dysphagia. Dysphagia, 28, 557-66.
Reason for exclusion: Quasi-experimental study design, not RCT.
Sukthankar S.M., Reddy N.P., Canilang E.P., Stephenson L., Thomas R. (1994). Design and development of portable biofeedback systems for use in oral dysphagia rehabilitation. Medical Engineering & Physics, 16, 430-435
Reason for exclusion: Population included other patients than those with stroke.
Takahata, H., Tsutsumi, K., Baba, H., Nagata, I., & Yonekura, M. (2011). Early intervention to promote oral feeding in patients with intracerebral hemorrhage: a retrospective cohort study. BMC neurology, 11(1), 1.
Reason for exclusion: Not RCT.
The FOOD Trial Collaboration. (2005). Effect of timing and method of enteral tube feeding for dysphagic stroke patients (FOOD): A multicentre randomised controlled trial. Lancet, 365, 764–72.
Reason for exclusion: Nature of the intervention is compensatory.
Theurer, J.A., Johnston, J.L., Fisher, J., Darling, S., Stevens, R.C., Taves, D., Teasell, R., Hachinski, V., & Martin, R.E. (2013). Proof-of-principle pilot study of oropharyngeal air-pulse application in individuals with dysphagia after hemispheric stroke. Archives of Physical Medicine and Rehabilitation, 94, 1088-94.
Reason for exclusion: Case-series study design, not RCT.
Whelan K. (2001). Inadequate fluid intakes in dysphagic acute stroke. Clinical Nutrition, 20(5), 423-428.
Reason for exclusion: Both groups received a form of the treatment.
Wada, S., Tohara, H., Iida, T., Inoue, M., Sato, M., & Ueda, K. (2012). Jaw-opening exercise for insufficient opening of the upper esophageal sphincter. Archives of Physical Medicine and Rehabilitation, 93, 1995-9.
Reason for exclusion: Other population than patients with stroke.



