Introduction
Functional electrical stimulation (FES), also called functional neuromuscular stimulation (FNS), is a technique used to replace or help a muscle contraction during a functional activity by applying electrical current to the nerves that control muscles. The goal of this treatment modality is to strengthen muscle contraction and improve motor control. The most familiar type of electrical stimulation is probably the use of pacemakers to control heart contractions.
Neuromuscular electrical stimulation, or simply ‘electrical stimulation’ (ES), is a modality used primarily for strengthening muscles, without the purpose of integrating a functional task as done with FES. Despite the use of all three terms in the literature (FES, FNS and ES), these modalities basically focus on eliciting muscular contractions.
This module summarizes the electrical stimulation modalities used to elicit muscular contraction of the upper extremities (FES of the shoulder is reviewed independently). Transcutaneous electrical nerve stimulation (TENS) and other therapeutic electrical stimulation that do not elicit muscular contraction are reviewed in other modules. The effectiveness of FES for improving functional independence/burden of care, strength, spasticity, range of motion, hand function, motor function and reaction time has been reported.
Patient/Family Information
What is functional electrical stimulation (FES)?
Functional electrical stimulation (FES) is a technique that causes a muscle to contract through the use of an electrical current. While this might sound strange, we should point out that the body naturally uses electrical current to make muscles move! Normally, when a part of the body needs to move, the brain sends electrical signals through the nervous system. The nerves, acting like electrical wires, relay these signals to the muscles, directing them to contract. This contraction causes the body part – for example, the elbow, wrist or finger joints – to move. After a stroke, some of these electrical signals do not function as well as they should.
When using FES as an intervention after a stroke, the therapist applies an electrical current to either the skin over the nerve, or over the bulk of the muscle, to cause a muscle contraction
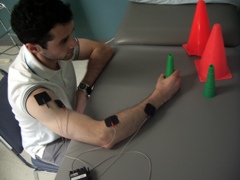
The idea behind FES is that this intervention allows the muscles that are paralyzed or partially paralyzed to move.
This module will look at the use of FES for loss of function, pain or spasticity (stiffness) of the arm, wrist and hand. Two other modules in StrokEngine focus on FES for the leg and on the shoulder. There is also an intervention using electrical stimulation that does not cause muscle contraction. This is called Transcutanious Electrical Neuromuscular Stimulation (TENS) and it is described in another module of StrokEngine (soon to come).
Are there different kinds of FES?
Yes, and you will see different names including: functional electrical stimulation, functional neuromuscular stimulation and electrical stimulation. But, they all have the same goal: to stimulate muscle contraction which in turn may lead to an increase in function, strength, and movement as well as a decrease in pain and spasticity. Also, FES may provide benefits such as increased reaction time and improved hand function (dexterity).
Why use FES for the arm and hand after stroke?
Loss of arm and hand function, movement, and strength are common after a stroke. Pain and spasticity are also common after a stroke. FES may be useful for increasing arm and hand function and for preventing pain and dysfunction after a stroke.
Does it work for stroke?
Researchers have studied how FES can help patients with stroke who experience a weak or painful hand.
- Hand function and dexterity: Both in acute and chronic individuals with stroke, researchers have found that FES is helpful in re-training hand function and dexterity.
- Functional independence: Research studies have shown that FES for the arm and hand were not effective in improving overall functional independence. In other words, patients who were treated with FES did not necessarily improve in their ability to take care of themselves.
- Strength: The research in this area is still inconclusive meaning we don’t know if FES is better than other treatments for strengthening the hand after a stroke.
- Spasticity (stiffness): There is limited evidence that FES reduces spasticity for patients in the chronic stroke phase.
- Range of motion (movement of joints): FES has not been shown to be effective for increasing movements of the hand and arm soon after a stroke (acute patients). But for clients who are in rehabilitation (in the sub-acute or chronic phases), FES applied to specific muscles has been shown to be more effective than regular therapy for increasing movement.
- Motor function (general functioning of muscles and nerves): There is conflicting evidence as to whether FES treatment, in combination with conventional physical therapy, can improve motor function in patients with acute stroke. However, for patients with sub-acute stroke, FES treatment combined with task specific exercises has been shown to improve motor function. For patients with chronic stroke, it has been shown that FES treatment in combination with conventional therapy does not improve motor function.
- Reaction time (how fast you move your hand in response to instructions): Researchers found that FES does help to improve reaction time in those with an acute stroke. But, for more chronic stroke patients, FES does not seem to be more beneficial than regular therapy.
What can I expect?
Small square stickers (electrodes) are placed over the centre of the bulk of the muscle. Wires connect the electrodes to a stimulator, a small machine that produces the current. The stimulation is usually started at a very low level causing a tingling “pins and needles” feeling on the skin. The current will then slowly be increased after each stimulation until it is strong enough to make the muscle contract. This level (the smallest current necessary to make the muscle contract) will be used for the treatment.


Although some people find the treatment uncomfortable, it is usually well tolerated because FES may give some discomfort, but it is virtually painless. Treatment times may vary. However, the time is usually divided into a number of daily sessions. FES treatments are usually done for 30 – 45 minutes, but once you are setup, you can typically perform the treatments on your own or with a family member.
Side effects/risks?
The electrodes can irritate the skin, but this is not common. Using non-latex hypoallergenic electrodes can often solve this problem. Some people may find that certain types of electrical stimulations are irritating, but this can be easily fixed by changing the level of the current. After the treatment, there may be pink marks left on the skin where the electrodes were placed, but these usually fade within an hour. Although very rare, this type of therapy can increase spasticity (muscle tightness).
Some people should not use FES.
NOTE: People with epilepsy, poor skin condition, hypersensitivity to the electrical stimulation, cancer, and cardiac pacemakers should not receive FES treatment.
Who provides the treatment?
Physical therapists or occupational therapists will usually provide the FES treatment. However, due to the long duration of the stimulation it is possible for the treatment to be done at home after discharge from the hospital. This will require having a stimulator at home. If it so happens that you are provided with a home stimulator, family members or friends will be given instructions on how to assist with treatments. Usually, once the electrodes are placed, the rest of the procedure is very simple.To operate an FES machine, you simply switching it on and increase (slowly and gradually) the intensity of the current on a knob – just like switching on a radio and increasing the volume.
NOTE: Consult with your therapist or medical professional on the exact use of specific models of FES equipment.
How many treatments?
Some patients continue to use FES for many years. To maximize the benefits after stroke, it should be used for at least 6 weeks.
How much does it cost? Does insurance pay for it?
Although the cost of an FES machine varies, some systems are relatively inexpensive. Rental or lease options bring the cost down to the equivalent of 1 or 2 clinical visits per month. Some insurance plans cover the purchase or rental of such equipment. Check with your insurance company.
Is FES for me?
While there have not been many high quality studies on FES for treating the arm and hand, those available generally report good overall results. More specifically, some studies on FES have reported it to be “ineffective” for independence in function, strength, spasticity or range of motion. These studies have compared FES to standard therapy. However, FES, when used on its own, does help recovery after stroke, although the differences between regular therapy and FES therapy might not have been large. There is clear evidence that there are benefits to using FES in comparison to regular therapy, including improved motor hand functioning and dexterity, and increased reaction times.
Clinician Information
Note: When reviewing the findings, it is important to note that they are always made according to randomized clinical trial (RCT) criteria – specifically as compared to a control group. To clarify, if a treatment is “effective” it implies that it is more effective than the control treatment to which it was compared. Non-randomized studies are no longer included when there is sufficient research to indicate strong evidence (level 1a) for an outcome.
Fourteen studies (12 RCTs, one non-RCT and one review article) have examined the efficacy of functional electrical stimulation (FES) as a means to improve hemiparetic upper extremity function post-stroke. Specifically, studies have investigated the effect of ES for improving muscle strength, spasticity, range of motion (ROM), motor function, manual dexterity, activities of daily living (ADL), reaction time and hand function post-stroke.
Results Table
View results table
Outcomes
Acute Phase
Functional independence
Not effective
1a
Three high quality RCTs (Mangold et al., 2009; Powell et al., 1999; Chae et al., 1998) have investigated the effectiveness of FES for improving functional independence in patients with acute stroke.
The first high quality RCT (Mangold et al., 2009) investigated the effectiveness of FES for improving functional independence in 23 patients with acute and sub-acute stroke. The participants were assigned to receive FES and conventional occupational therapy or conventional therapy only. Both groups received 45 minutes of occupational therapy, 3 to 5 times per week for 4 weeks, where the intervention group replaced 3 of their sessions with FES. Outcomes were measured at post-treatment and at six months. At post-treatment there was a significant difference between the groups in favour of the stimulation group on the Extended Barthel Index. Scores were not reported at the six month follow-up.
The second high quality RCT (Powell et al., 1999) investigated the use of FES for improving functional independence in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, 3 times a week for 8 weeks. Outcomes were measured at eight weeks and a 32 week follow-up. At eight weeks and at a 32 week follow-up, there were no significant between group differences on the Barthel Index or the Rankin scale.
The third high quality RCT (Chae et al., 1998) investigated the effectiveness of FES for improving functional independence in 46 patients with acute stroke. The participants were randomized to receive either FES to produce wrist and finger extension exercises or sham stimulation (control group). The sessions were 1 hour a day for 15 sessions (3 weeks). Outcomes were measured at post-treatment (four weeks) and at a 12 week follow-up. At both the four and 12 week assessment, there were no significant between group differences on the Functional Independence Measure (FIM).
Conclusion: There is strong evidence (Level 1a) from two high quality RCTs that FES in combination with conventional therapy is not more effective than conventional therapy (alone or in combination with sham stimulation) for improving functional independence in patients with acute stroke.
Note: However, one high quality RCT found a significant difference between the groups in favour of the stimulation group on the Extended Barthel Index but scores were not reported at the six month follow-up.
Hand function and dexterity
Effective
1B
One high quality RCT (Powell et al., 1999) and one fair quality RCT (Alon et al., 2008) have investigated the effectiveness of FES for improving hand function and dexterity in patients with acute stroke.
The high quality RCT (Powell et al., 1999) investigated the use of FES for improving hand function and dexterity in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, 3 times a week for 8 weeks. Outcomes were measured at eight weeks and at 32 weeks. At post-treatment (eight weeks) there was a significant difference in favour of the stimulation group on hand function and dexterity measured on the grip and grasp items of the Action Research Arm test. This difference was not maintained at the 32 week follow-up.
The fair quality RCT (Alon et al., 2008) investigated the effectiveness of FES for improving hand function and dexterity in 26 patients with acute stroke. The participants were assigned to receive either FES in combination with task-specific exercise or task-specific exercise only. Sessions were given 2 times/day for 30 minutes, 5 days/week for 12 weeks. The FES group practiced the exercises while receiving FES as well as received additional FES without exercises for up to an additional 90 minutes twice a day. Outcomes were measured at baseline and at 12 weeks. At 12 weeks, there were no significant between group differences on hand function and dexterity, measured by the Box and Blocks test, or the Jebsen-Taylor light object lift test.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that FES in addition to conventional therapy is more effective than conventional therapy only for improving hand function and dexterity in patients with acute stroke. However these improvements were not maintained in the long-term.
Note: However, one fair quality RCT did not find any significant between group differences on hand function and dexterity.
Motor function
Not effective
1A
Three high quality RCTs (Mangold et al., 2009; Powell et al., 1999.; Chae et al., 1998) and one fair quality RCT (Alon et al., 2008) have investigated the effectiveness of FES for improving motor function in patients with acute stroke.
The first high quality RCT (Mangold et al., 2009) investigated the effectiveness of FES for improving motor function in 23 patients with acute and sub-acute stroke. The participants were assigned to receive FES and conventional occupational therapy or conventional therapy only. Both groups received 45 minutes of occupational therapy, 3 to 5 times per week for 4 weeks, where the intervention group replaced 3 of their sessions with FES. Outcomes were measured at post-treatment (four weeks). At post-treatment there was no significant difference between the groups on the Chedoke McMaster Stroke Assessment. Scores at the six month follow-up were not reported.
The second high quality RCT ( Powell et al., 1999) investigated the effectiveness of FES for improving motor function in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, three times a week for eight weeks. Outcomes were measured at eight weeks and at a 32 week follow-up. At post treatment (8 weeks) and at the 32 week follow-up, there were no significant between group differences on the Nine-hole peg test.
The third high quality RCT ( Chae et al., 1998) investigated the effectiveness of FES for improving motor function in 46 patients with acute stroke. The participants were randomized to receive either FES to produce wrist and finger extension exercises or sham stimulation (control group). The sessions were 1 hour a day for 15 sessions (3 weeks). Outcomes were measured at four weeks and at 12 weeks. At post-treatment, there was a significant between group difference in favour of the experimental group on the Fugl-Meyer Assessment, however, this difference was not maintained at the 12 week follow-up.
The fair quality RCT (Alon et al., 2008) investigated the effectiveness of FES for improving motor function in 26 patients with acute stroke. The participants were assigned to receive either FES in combination with task-specific exercise or task-specific exercise only. Sessions were given 2 times/day for 30 minutes, 5 days/week for 12 weeks. The FES group practiced the exercises while receiving FES as well as received additional FES without exercises for up to an additional 90 minutes twice a day. Outcomes were measured at post-treatment (12 weeks). At post-treatment, there was a significant between group difference on the upper extremity section of the modified Fugl-Meyer Assessment in favour of the experimental group.
Conclusion: There is strong evidence (Level 1a) from two high quality RCTs that FES in addition to conventional therapy or no therapy is not more effective than conventional therapy or no therapy alone for improving motor function in patients with acute stroke.
Note: However, one high quality RCT and one fair quality RCT found a significant difference between the groups in favour of the stimulation group (this difference was not maintained at the 12 week follow-up for the high quality RCT).
Range of motion
Not effective
1B
One high quality RCT (Powell et al., 1999) has investigated the effectiveness of FES for improving range of motion in patients with acute stroke.
The high quality RCT (Powell et al., 1999) investigated the effectiveness of FES for improving range of motion in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, 3 times a week for 8 weeks. Outcomes were measured at eight weeks, and at a 32 weeks follow-up. At post-treatment and at the 32 week follow-up, there were no significant between group differences on passive and active range of motion.
Conclusion: There is moderate evidence (Level 1b) from one high RCT that FES in addition to conventional therapy is not more effective than conventional therapy alone for improving range of motion in patients with acute stroke.
One high quality RCT (Powell et al., 1999) has investigated the effectiveness of FES for improving reaction time in patients with acute stroke.
The high quality RCT (Powell et al., 1999) investigated the effectiveness of FES for improving reaction time in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, 3 times a week for 8 weeks. Outcomes were measured at post-treatment (eight weeks) and at a 32 weeks. At post-treatment and at the 32 week follow-up, there was a significant difference between the groups in favour of the experimental group on reaction time.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that FES in addition to conventional therapy is more effective than conventional therapy only for improving reaction time in patients with acute stroke.
Spasticity
Not effective
1A
Two high quality RCTs (Mangold et al., 2009, Powell et al., 1999) have investigated the effectiveness of FES for improving spasticity in patients with acute stroke.
The first high quality RCT (Mangold et al., 2009) investigated the effectiveness of FES for improving spasticity in 23 patients with acute and sub-acute stroke. The participants were assigned to receive FES and conventional occupational therapy or conventional therapy only. Both groups received 45 minutes of occupational therapy, 3 to 5 times per week for 4 weeks, where the intervention group replaced 3 of their sessions with FES. Outcomes were measured at four weeks. At post-treatment, there was no significant between group difference on the Modified Ashworth Scale. Scores at the six month follow-up were not reported.
The second high quality RCT (Powell et al., 1999) investigated the effectiveness of FES for improving spasticity in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, 3 times a week for 8 weeks. Outcomes were measured at eight weeks and at a 32 week follow-up. At post-treatment and at the 32 week follow-up, there was no significant difference in spasticity between the groups measured by the Modified Ashworth Scale.
Conclusion: There is strong evidence (Level 1a) from two high quality RCTs that FES in addition to conventional therapy is not more effective than conventional therapy alone for improving spasticity in patients with acute stroke.
One RCT (Powell et al., 1999) has investigated the effectiveness of FES for improving strength in patients with acute stroke.
The high quality RCT (Powell et al., 1999) investigated the effectiveness of FES for improving strength in 60 patients with acute stroke. The participants were assigned to receive either FES in addition to conventional (Bobath) therapy or conventional (Bobath) therapy only. Sessions were given for 30 mins/day, 3 times a week for 8 weeks. Outcomes were measured at eight weeks, and at a 32 weeks follow-up. At post-treatment and at a 32 week follow-up, there was no significant difference in grip strength between the groups.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that FES in addition to conventional therapy is not more effective than conventional therapy alone for improving strength in patients with acute stroke.
Subacute Phase
Functional independence
Effective
1b
One high quality RCT (Francisco et al., 1998) has investigated the effectiveness of FES for improving functional independence in patients with sub-acute stroke.
The high quality RCT (Francisco et al., 1998) investigated the effectiveness of FES for improving functional independence in 9 patients with sub-acute stroke. The participants were assigned to receive either EMG-triggered FES in combination with conventional therapy or conventional therapy only. The sessions were 30 minutes a day, 5 days a week for the duration of the participants stay in the hospital. Outcomes were measured at the end of each participants hospital stay. At post-treatment there was a significant difference in favour of the experimental group on the self-care items of the Functional Independence Measure (FIM).
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that EMG-triggered FES in combination with conventional therapy is more effective than conventional therapy alone for improving functional independence in patients with sub-acute stroke.
Hand function and dexterity
Not effective
2A
One fair quality RCT (Hemmen & Seelen, 2007) has investigated the effectiveness of FES for improving hand function and dexterity in patients with sub-acute stroke.
The fair quality RCT (Hemmen & Seelen, 2007) investigated the effectiveness of FES for improving hand function and dexterity in 27 patients with sub-acute stroke. The participants were assigned to receive either movement imagery-assisted electromyography (EMG)-triggered feedback, or electrostimulation. Both groups received their treatments for 30 minutes a day, 5 days a week for 12 weeks in addition to conventional therapy. Outcomes were measured at post-treatment (three months) and at a 12 month follow-up. A significant increase in arm-hand function within each group was found at post-treatment and at the 12 month follow-up within each group, however, there was no significant difference found between the groups on the Action Research Arm Test.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that imagery-assisted electromyography (EMG)-triggered feedback in combination with conventional therapy is not more effective than electrostimulation in combination with conventional therapy for improving hand function and dexterity in patients with sub-acute stroke.
Motor function
Effective
1B
One high quality RCT (Francisco et al., 1998) and one fair quality RCT (Hemmen & Seelen, 2007) have investigated the effectiveness of FES for improving motor function in patients with sub-acute stroke.
The high quality RCT (Francisco et al., 1998) investigated the effectiveness of FES for improving motor function in 9 patients with sub-acute stroke. The participants were assigned to receive either EMG-triggered FES in combination with conventional therapy or conventional therapy only. The sessions were 30 minutes a day, 5 days a week for the duration of the participants stay in the hospital. Outcomes were measured at the end of each participants hospital stay. At post-treatment there was a significant difference in favour of the experimental group on the upper limb section of the Fugl-Meyer Assessment.
The fair quality RTC (Hemmen & Seelen, 2007) investigated the effectiveness of FES for improving hand function and dexterity in 27 patients with sub-acute stroke. The participants were assigned to receive either movement imagery-assisted electromyography (EMG)-triggered feedback, or electrostimulation. Both groups received their treatments for 30 minutes a day, 5 days a week for 12 weeks in addition to conventional therapy. Outcomes were measured at post-treatment (three months) and at a 12 week follow-up. At post-treatment and at a 12 month follow-up, there was no significant difference found between the groups on the Brunnstrom Fugl-Meyer.
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that EMG-triggered FES in addition to conventional therapy is more effective than conventional therapy alone for improving motor function in patients with sub-acute stroke.
Note: However, one fair quality RCT did not find any significant between group differences on motor function.
Range of motion
Effective
2a
One fair quality RCT (Bowman et al., 1979) has investigated the effectiveness of FES for improving range of motion in patients with sub-acute stroke.
The fair quality RCT (Bowman et al., 1979) investigated the effectiveness of FES for improving range of motion in 30 patients with sub-acute stroke. The participants were assigned to receive either positional feedback stimulation in addition to conventional therapy, or conventional therapy only. Sessions were 30 minutes a day, 5 days a week, for 4 weeks. Outcomes were measured at post-treatment (four weeks). At post-treatment, there was a significant difference in favour of the group receiving positional feedback stimulation in addition to conventional therapy on selective range of motion.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that positional feedback stimulation in addition to conventional therapy is more effective than conventional therapy alone for improving range of motion in patients with sub-acute stroke.
Chronic Phase
Electromyographic measures
Effective
2a
One fair quality RCT (Hara et al., 2008) has investigated the effectiveness of FES for improving electromyographic measures in patients with chronic stroke.
The fair quality RCT (Hara et al., 2008 ) investigated the effectiveness of daily power-assisted FES for improving electromyographic measures in 20 patients with chronic stroke. The experimental group received, at home, power-assisted FES and standard therapy, and the control group received standard therapy alone. The FES treatment was conducted for 1 hour a day for 5 months. Standard therapy was received once a week for 40 minutes over the 5 months. Outcomes were assessed at post-treatment (5 months). At post-treatment there was a statistically significant between-group difference in favor of the group receiving FES on electromyographic measures.
Conclusion: There is limited evidence (Level 2a) from one fair quality RCT that power-assisted FES in combination with conventional therapy is more effective than conventional therapy alone for improving electromyographic measures in patients with chronic stroke.
Functional independence
Not effective
1b
One high quality RCT (Chan et al., 2009) has investigated the effectiveness of FES for improving functional independence in patients with chronic stroke.
The high quality RCT (Chan et al., 2009) has investigated the effectiveness of FES for improving functional independence in 20 patients with chronic stroke. The participants were assigned to receive either FES in combination with bilateral upper limb motor training and conventional therapy, or bilateral upper limb training and conventional therapy only. 15 sessions were given, each one 20 minutes in length. Each session was preceded by 10 minutes of stretching and followed by 60 minutes of conventional occupational therapy. Outcomes were measured at the end of the 15 sessions. At post-treatment there was no difference between the groups on the Functional Independence Measure (FIM).
Conclusion: There is moderate evidence (Level 1b) from one high quality RCT that FES in combination with bilateral motor training and conventional therapy is not more effective than bilateral motor training and conventional therapy only for improving functional independence in patients with chronic stroke.
Hand function and dexterity
Effective
1A
One meta-analysis (Bolton et al., 2004), two high quality RCTs ( Cauraugh & Kim, 2003a , Cauraugh & Kim, 2003b ) and three fair quality RCTs ( Cauraugh et al., 2000 , Cauraugh & Kim, 2002 , Hara et al., 2008) have investigated the effectiveness of FES for improving hand function and dexterity in patients with chronic stroke.
The meta-analysis (Bolton et al., 2004) examined five studies to assess the effect of EMG-triggered neuromuscular stimulation on arm and hand function post-stroke. 84% of the patient population were in the chronic stage of recovery, and the remainder were acute and sub-acute. The total number of individuals studied was 47 in the treatment groups and 39 in the control groups. Subjects in the control group received usual stroke therapy (i.e. ROM stretching, neuromuscular facilitation, and functional training of the affected upper extremity). Overall, there was a significant difference between the patients treated with FES compared to those that received conventional therapy on the Box and Blocks Test.
The first high quality RCT (Cauraugh & Kim, 2003a) investigated the effectiveness of FES for improving hand function and dexterity in 26 patients with chronic stroke. The participants were assigned to receive 1) 0 seconds of active neuromuscular stimulation (control group), 2) 5 seconds of active neuromuscular stimulation or 3) 10 seconds of neuromuscular stimulation applied to the back of the impaired forearm. In addition, all participants received bilateral movement training. All participants completed 4 days (90 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 3 sets of 30 active neuromuscular stimulation trials (either 0, 5 or 10 sec depending on group assignment) along with 3 sets of 30 bilateral extension movements of the hand. At post-treatment, there was a significant difference between the 10 second group and the 5 second group on the number of blocks moved on the Box and Blocks Test.
The second high quality RCT (Cauraugh & Kim, 2003b) investigated the effectiveness of FES for improving hand function and dexterity in 34 patients with chronic stroke. The participants were assigned to receive 1) blocked practice (repetitive movements) in combination with active neuromuscular stimulation; (2) random practice (different movements) in combination with active stimulation; or (3) no active neuromuscular stimulation intervention (control). Extension of the wrist/fingers joint, elbow joint, and shoulder joint were performed by all subjects for 2, 90-minute sessions a week for a period of 2 weeks. At post-treatment there was a significant difference between the blocked practice group and the control group, in favour of the blocked practice group, and between the random practice group and the control group (in favour of the random practice group) on the number of blocks moved on the Box and Blocks Test.
The first fair quality RCT (Cauraugh et al., 2000) investigated the effectiveness of FES for improving hand function and dexterity in 11 patients with chronic stroke. The participants were assigned to receive 1) electrical stimulation during voluntary extension of the wrist/fingers, 2) voluntary extension of the wrist/fingers alone. Both groups received passive range of motion (ROM) and stretching exercises prior to the treatment. All participants completed 3 days (60 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 2 sets of 30 active neuromuscular stimulation trials. The control group also performed voluntary extension of the wrist/fingers for 60 minutes per day (2 sets of 30 movements). At post-treatment, there was a significant difference in favour of the stimulation group on the number of blocks moved on the Box and Blocks Test.
The second fair quality RCT (Cauraugh & Kim, 2002) investigated the effectiveness of FES for improving hand function and dexterity in 25 patients with chronic stroke. The participants were assigned to receive 1) EMG-triggered stimulation and bilateral movement, 2) EMG-triggered stimulation and unilateral movement or 3) a control group that performed wrist and finger exercises only. All participants completed 4 days (90 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 3 sets of 30 active neuromuscular stimulation trials along with either bilateral or unilateral training (extensions of the wrist/fingers); the control group executed 90 voluntary wrist/finger extensions of the impaired hand per session without active stimulation. At post-treatment, there was a significant difference in favour of the stimulation and bilateral training group compared to the stimulation and unilateral training group and the control group on the number of blocks moved on the Box and Blocks Test. There was also a significant difference between the stimulation and unilateral training group compared to the control group on the number of blocks moved on the Box and Blocks Test.
The third fair quality RCT (Hara et al., 2008) investigated the effectiveness of FES for improving hand function and dexterity in 20 patients with chronic stroke. The experimental group received, at home, power-assisted FES and standard therapy, and the control group received standard therapy alone. The FES treatment was conducted for 1 hour a day for 5 months. Standard therapy was received once a week for 40 minutes over the 5 months. At post-treatment, there was a significant difference in favour of the FES group compared to the control group on both the 10 Cup Moving Test & Nine-Hole-Peg Test.
Conclusion: There is strong evidence (level 1a) from one meta-analysis, two high quality RCTs and three fair quality RCTs that FES in combination with conventional therapy or training is more effective than conventional therapy or training only for improving hand function and dexterity in patients with chronic stroke.
Motor function
Effective
1A
One meta-analysis (Bolton et al., 2004), one high quality RCT ( Chan et al., 2009 ), one fair quality RCT (Cauraugh et al., 2000) and one pre-post study (Gritsenko & Prochazka, 2004) have investigated the effectiveness of FES for improving motor function in patients with chronic stroke.
The meta-analysis (Bolton et al., 2004) examined five studies to assess the effect of EMG-triggered neuromuscular stimulation on arm and hand function post-stroke. 84% of the patient population were in the chronic stage of recovery, and the remainder were acute and sub-acute. The total number of individuals studied was 47 in the treatment groups and 39 in the control groups. Subjects in the control group received usual stroke therapy (i.e. ROM stretching, neuromuscular facilitation, and functional training of the affected upper extremity). Overall, there was a significant difference between the patients treated with FES compared to those that received conventional therapy on the Fugl-Meyer Assessment, Box and Blocks Test and the Rivermead Motor Assessment.
The high quality RCT (Chan et al., 2009) has investigated the effectiveness of FES for improving motor function in 20 patients with chronic stroke. The participants were assigned to receive either FES in combination with bilateral upper limb motor training and conventional therapy, or bilateral upper limb training and conventional therapy only. 15 sessions were given, each one 20 minutes in length. Each session was preceded by 10 minutes of stretching and followed by 60 minutes of conventional occupational therapy. Outcomes were measured after the 15 sessions. At post-treatment there was a significant difference between the groups in favour of the stimulation group on the Functional Test for the Hemiplegic Upper Limb (FTHUE) and on the Fugl-Meyer Assessment.
The fair quality RCT (Cauraugh et al., 2000) investigated the effectiveness of FES for improving motor function in 11 patients with chronic stroke. The participants were assigned to receive 1) electrical stimulation during voluntary extension of the wrist/fingers, 2) voluntary extension of the wrist/fingers alone. Both groups received passive range of motion (ROM) and stretching exercises prior to the treatment. All participants completed 3 days (60 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 2 sets of 30 active neuromuscular stimulation trials. The control group also performed voluntary extension of the wrist/fingers for 60 minutes per day (2 sets of 30 movements). Outcomes were measured at post-treatment (two weeks). At post-treatment there was no significant difference between the groups on the Fugl-Meyer Assessment and the Motor Assessment Scale.
The pre-post study (Gritsenko & Prochazka, 2004) investigated the effectiveness of FES for improving motor function in 6 patients with chronic stroke. The participants received FES-assisted exercise therapy (reaching, grasping and moving) for 12 sessions of one hour each. Outcomes were measured at post-treatment (after 12 sessions) and at a two month follow-up. At post-treatment and at the two month follow-up, there were no significant improvements on the Fugl-Meyer Assessment and Motor Activity Log, however, these patients did show significant improvements between pre-and post-assessment on the Wolf Motor Function Test following therapy.
Conclusion: There is strong evidence (level 1a) from one meta-analysis and one high quality RCT that FES in combination with voluntary movement, bilateral motor training or conventional therapy is more effective than bilateral motor training or conventional therapy only for improving motor function in patients with chronic stroke.
Note: However, one fair quality RCT did not find any significant between group differences on the Fugl-Meyer Assessment and the Motor Assessment Scale.
Range of motion
Effective
1B
One high quality RCT (Chan et al., 2009) and one fair quality RCT (Hara et al., 2008) has investigated the effectiveness of FES for improving range of motion in patients with chronic stroke.
The high quality RCT (Chan et al., 2009) has investigated the effectiveness of FES for improving range of motion in 20 patients with chronic stroke. The participants were assigned to receive either FES in combination with bilateral upper limb motor training and conventional therapy, or bilateral upper limb training and conventional therapy only. 15 sessions were given, each one 20 minutes in length. Each session was preceded by 10 minutes of stretching and followed by 60 minutes of conventional occupational therapy. Outcomes were measured after 15 sessions. At post-treatment there was a significant difference in favour of the stimulation group on active range of motion of the wrist, however no difference was found between the groups on forward reaching distance.
The fair quality RCT (Hara et al., 2008) investigated the effectiveness of FES for improving range of motion in 20 patients with chronic stroke. The experimental group received, at home, power-assisted FES and standard therapy, and the control group received standard therapy alone. The FES treatment was conducted for one hour a day for five months. Standard therapy was received once a week for 40 minutes over the five months. Outcomes were measured at post-treatment (five months). At post-treatment, there was a significant difference in favour of the stimulation group on measures of range of motion (measured by goniometry).
Conclusion: There is moderate evidence (level 1b) from one high quality and one fair quality RCT that FES in addition to bilateral motor training or conventional therapy is more effective than bilateral motor training or conventional therapy only for improving active range of motion in patients with chronic stroke.
Reaction time
Conflicting
4
Two high quality RCTs (Cauraugh & Kim, 2003a, Cauraugh & Kim, 2003b) and two fair quality RCTs (Cauraugh et al., 2000; Cauraugh & Kim, 2002) have investigated the effectiveness of FES for improving reaction time in patients with chronic stroke.
The first high quality RCT (Cauraugh & Kim, 2003a) investigated the effectiveness of FES for improving reaction time in 26 patients with chronic stroke. The participants were assigned to receive 1) 10 seconds of neuromuscular stimulation applied to the back of the impaired forearm, 2) 5 seconds of active neuromuscular stimulation or 3) 0 seconds of active neuromuscular stimulation (control group). In addition, all participants received bilateral movement training. All participants completed 4 days (90 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 3 sets of 30 active neuromuscular stimulation trials (either 0, 5 or 10 sec depending on group assignment) along with 3 sets of 30 bilateral extension movements of the hand. Outcomes were measured at post-treatment (two weeks). At post-treatment, there were no significant differences between the groups on reaction time.
The second high quality RCT (Cauraugh & Kim, 2003b) investigated the effectiveness of FES for improving reaction time in 34 patients with chronic stroke. The participants were assigned to receive 1) blocked practice (repetitive movements) in combination with active neuromuscular stimulation; (2) random practice (different movements) in combination with active stimulation; or (3) no active neuromuscular stimulation intervention (control). Extension of the wrist/fingers joint, elbow joint, and shoulder joint were performed by all subjects for 2, 90-minute sessions a week for a period of two weeks. At post-treatment (two weeks) there was a significant difference between in favour of the two stimulation groups compared to the control group on reaction time. No significant difference was found between the blocked and random practice stimulation groups.
The first fair quality RCT (Cauraugh et al., 2000 investigated the effectiveness of FES for improving reaction time in 11 patients with chronic stroke. The participants were assigned to receive 1) electrical stimulation during voluntary extension of the wrist/fingers, 2) voluntary extension of the wrist/fingers alone. Both groups received passive range of motion (ROM) and stretching exercises prior to the treatment. All participants completed 3 days (60 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 2 sets of 30 active neuromuscular stimulation trials. The control group also performed voluntary extension of the wrist/fingers for 60 minutes per day (2 sets of 30 movements). Outcomes were measured at post-treatment (2 weeks). At post-treatment there were no significant differences between the groups on reaction time.
The second fair quality RCT (Cauraugh & Kim, 2002) investigated the effectiveness of FES for improving reaction time in 25 patients with chronic stroke. The participants were assigned to receive 1) EMG-triggered stimulation and bilateral movement, 2) EMG-triggered stimulation and unilateral movement or 3) a control group that performed wrist and finger exercises only. All participants completed 4 days (90 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 3 sets of 30 active neuromuscular stimulation trials along with either bilateral or unilateral training (extensions of the wrist/fingers); the control group executed 90 voluntary wrist/finger extensions of the impaired hand per session without active stimulation. Outcomes were measured at post-treatment (two weeks). At post-treatment there was a significant difference in favour of the two stimulation groups compared to the control group on reaction time.
Conclusion: There is conflicting evidence (Level 4) from two high quality RCTs and two fair quality RCTs of whether FES in combination with conventional therapy or training is more effective than conventional therapy or training alone for improving reaction time in patients with chronic stroke.
Note: These studies have small sample sizes which may, in part, be contributing to the divergent findings.
Spasticity
Not effective
1B
One high quality RCT ( Chan et al., 2009 ) and one fair quality RCT (Hara et al., 2008) have investigated the effectiveness of FES for improving spasticity in patients with chronic stroke.
The high quality RCT (Chan et al., 2009) has investigated the effectiveness of FES for improving spasticity in 20 patients with chronic stroke. The participants were assigned to receive either FES in combination with bilateral upper limb motor training and conventional therapy, or bilateral upper limb training and conventional therapy only. 15 sessions were given, each one 20 minutes in length. Each session was preceded by 10 minutes of stretching and followed by 60 minutes of conventional occupational therapy. Outcomes were measured after the 15 sessions. At post-treatment there was no significant difference between the groups on the Modified Ashworth Scale.
The fair quality RCT (Hara et al., 2008) investigated the effectiveness of FES for improving spasticity in 20 patients with chronic stroke. The experimental group received, at home, power-assisted FES and standard therapy, and the control group received standard therapy alone. The FES treatment was conducted for 1 hour a day for five months. Standard therapy was received once a week for 40 minutes over the five months. Outcomes were measured at post-treatment (five months). At post-treatment, there was a significant difference between the groups in favour of the stimulation group on the Modified Ashworth Scale.
Conclusion: There is moderate evidence (level 1b) from one high quality RCT that FES in addition to bilateral motor training or conventional therapy is not more effective than bilateral motor training or conventional therapy only for improving spasticity in patients with chronic stroke.
Note: However, one fair quality RCT found a significant difference between the groups in favour of the stimulation group on the Modified Ashworth Scale.
One meta-analysis (Glanz et al., 1996), three high quality RCTs ( Chan et al., 2009 ; Cauraugh & Kim, 2003a; Cauraugh & Kim, 2003b) and two fair quality RCTs (Cauraugh et al., 2000; Cauraugh & Kim, 2002) have investigated the effectiveness of FES for improving strength in patients with chronic stroke.
The meta-analysis (Glanz et al., 1996) examined four randomized controlled trials to assess the effectiveness of functional electrical stimulation (FES) therapy for improving muscular strength in patients with chronic stroke. The range of mean time since onset of symptoms for the individuals in the four studies included was 1.5 months to 29.2 months. The treatment group received FES for a muscle in their hemiparetic extremity (ankle, knee or wrist), along with standard physical therapy. The control group received physical therapy alone for all studies except one, where these patients received a sham treatment. All four studies generated a positive effect size (0.63), where patients who received FES had significant improvements in muscle strength of the hemiparetic extremity (ankle, knee or wrist) at post-treatment, in comparison to those who received standard physical therapy or even a sham treatment.
The first high quality RCT (Chan et al., 2009) has investigated the effectiveness of FES for improving strength in 20 patients with chronic stroke. The participants were assigned to receive either FES in combination with bilateral upper limb motor training and conventional therapy, or bilateral upper limb training and conventional therapy only. 15 sessions were given, each one 20 minutes in length. Each session was preceded by 10 minutes of stretching and followed by 60 minutes of conventional occupational therapy. Outcomes were measured after the 15 sessions. At post-treatment there was no difference between the groups on grip power.
The second high quality RCT (Cauraugh & Kim, 2003a) investigated the effectiveness of FES for improving strength in 26 patients with chronic stroke. The participants were assigned to receive 1) 0 seconds of active neuromuscular stimulation (control group), 2) 5 seconds of active neuromuscular stimulation or 3) 10 seconds of neuromuscular stimulation applied to the back of the impaired forearm. In addition, all participants received bilateral movement training. All participants completed 4 days (90 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 3 sets of 30 active neuromuscular stimulation trials (either 0, 5 or 10 sec depending on group assignment) along with 3 sets of 30 bilateral extension movements of the hand. Outcomes were measured at two weeks. At post-treatment there were no significant differences between the groups on sustained contraction of wrist extension.
The third high quality RCT (Cauraugh & Kim, 2003b) investigated the effectiveness of FES for improving strength in 34 patients with chronic stroke. The participants were assigned to receive 1) blocked practice (repetitive movements) in combination with active neuromuscular stimulation; (2) random practice (different movements) in combination with active stimulation; or (3) no active neuromuscular stimulation intervention (control). Extension of the wrist/fingers joint, elbow joint, and shoulder joint were performed by all subjects for 2, 90-minute sessions a week for a period of 2 weeks. Outcomes were measured at two weeks. At post-treatment there was a significant difference in favour of both stimulation groups compared to the control group on sustained contraction of wrist extension.
The first fair quality RCT (Cauraugh et al., 2000) investigated the effectiveness of FES for improving strength in 11 patients with chronic stroke. The participants were assigned to receive 1) electrical stimulation during voluntary extension of the wrist/fingers, 2) voluntary extension of the wrist/fingers alone. Both groups received passive range of motion (ROM) and stretching exercises prior to the treatment. All participants completed 3 days (60 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 2 sets of 30 active neuromuscular stimulation trials. The control group also performed voluntary extension of the wrist/fingers for 60 minutes per day (2 sets of 30 movements). Outcomes were measured at post-treamtent (two weeks). At post-treatment there was a significant difference between the groups in favour of the stimulation group on sustained contraction of wrist extension.
The second fair quality RCT (Cauraugh & Kim, 2002) investigated the effectiveness of FES for improving strength in 25 patients with chronic stroke. The participants were assigned to receive 1) EMG-triggered stimulation and bilateral movement, 2) EMG-triggered stimulation and unilateral movement or 3) a control group that performed wrist and finger exercises only. All participants completed 4 days (90 minutes per day) of rehabilitation training over a 2-week period. Each session consisted of 3 sets of 30 active neuromuscular stimulation trials along with either bilateral or unilateral training (extensions of the wrist/fingers); the control group executed 90 voluntary wrist/finger extensions of the impaired hand per session without active stimulation. Outcomes were measured at post-treatment (two weeks). At post-treatment, there were no significant differences between the groups on sustained contraction of wrist extension.
Conclusion: There is strong evidence (level 1a) from one meta-analysis, one high quality RCT and one fair quality RCT that FES in addition to bilateral motor training or conventional therapy is more effective than bilateral training or conventional therapy alone for improving strength in patients with chronic stroke.
Note: However, two high quality RCTs and one fair quality RCT did not find any significant between group differences on the grip power or the sustained contraction of wrist extension.
References
Alon G., Levitt A.F., McCarthy P.A., Alan F. (2008). Functional electrical stimulation (FES) may modify the poor prognosis of strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. survivors with severe motor loss of the upper extremity: a preliminary study. American Journal of Physical Medicine and Rehabilitation, 87(8), 627-636.
Bolton D. A., Cauraugh J. H., & Hausenblas, H. A. (2004). Electromyogram-triggered neuromuscular stimulation and strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. motor recovery of arm/hand functions: a meta-analysisMethod in which the results of two or more studies are statistically combined. Typically used when studies have few subjects, but similar designs. By increasing the available number of subjects, more weight can be given to the findings.
. J Neurol Sci, 223(2), 121-127.
Bowman B. R., Baker L. L., & Waters, R. L. (1979). Positional feedback and electrical stimulation: an automated treatment for the hemiplegic wrist. Arch Phys Med Rehabil, 60(11), 497-502.
Cauraugh J. H., & Kim, S. (2002). Two coupled motor recovery protocols are better than one: electromyogram-triggered neuromuscular stimulation and bilateral movements. StrokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain., 33(6), 1589-1594.
Cauraugh J. H., & Kim, S. B. (2003a). Chronic strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. motor recovery: duration of active neuromuscular stimulation. J Neurol Sci, 215(1-2), 13-19.
Cauraugh J. H., & Kim, S. B. (2003b). StrokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. motor recovery: Active neuromuscular stimulation and repetitive practice schedules. J Neurol Neurosurg Psychiatry, 74(11), 1562-1566.
Cauraugh J. H., Kim S. B., & Duley, A. (2005). Coupled bilateral movements and active neuromuscular stimulation: intralimb transfer evidence during bimanual aiming. Neurosci Lett, 382(1-2), 39-44.
Cauraugh J., Light K., Kim S., Thigpen M., & Behrman, A. (2000). Chronic motor dysfunction after strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain.: recovering wrist and finger extension by electromyography-triggered neuromuscular stimulation. StrokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain., 31(6), 1360-1364.
Chae J, Bethoux F, Bohine T, Dobos L, Davis T, Friedl A. Neuromuscular stimulation for upper extremity motor and functional recovery in acute hemiplegiaComplete paralysis of the arm, leg, and trunk on one side of the body that results from damage to the parts of the brain that control muscle movements. Hemiplegia is not a progressive condition, nor is it a disease.. StrokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. 1998; 29(5): 975-979.
Chan M.K.L., Tong R.K.Y., Chung K.Y.K. (2009). Bilateral upper limb raining with functional electric stimulation in patients with chronic strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain.. Neurorehabilitation and Neural Repair, 23(4), 357-365.
Francisco G., Chae J., Chawla H., Kirshblum S., Zorowitz R., Lewis G., et al. (1998). Electromyogram-triggered neuromuscular stimulation for improving the arm function of acute strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. survivors: a randomized pilot study. Arch Phys Med Rehabil, 79(5), 570-575.
Glanz M., Klawansky S., Stason W., Berkey C., & Chalmers, T. C. (1996). Functional electrostimulation in poststroke rehabilitation: a meta-analysisMethod in which the results of two or more studies are statistically combined. Typically used when studies have few subjects, but similar designs. By increasing the available number of subjects, more weight can be given to the findings.
of the randomized controlled trials. Arch Phys Med Rehabil, 77(6), 549-553.
Gritsenko V., & Prochazka, A. (2004). A functional electric stimulation-assisted exercise therapy system for hemiplegic hand function. Arch Phys Med Rehabil, 85(6), 881-885.
Hara Y., Ogawa S., Tsujiuchi K., & Muraoka Y. (2008). A home-based rehabilitation program for the hemiplegic upper extremity by power-assisted functional electrical stimulation. Disability and Rehabilitation, 30, 296-304.
Hemmen B., Seelen H.A.M. (2007). Effects of movement imagery and electromyography-triggered feedback on arm-hand function in strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. patients in the sub-acute phase. Clinical Rehabilitation, 21, 587-594.
Mangold S, Schuster C, Keller T, Zimmermann-Schlatter A, Ettlin T. (2009). Motor training of upper extremity with functional electrical stimulation in early strokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain. rehabilitation. Neurorehabil Neural Repair, 23(2): 184-90.
Powell J., Pandyan A. D., Granat M., Cameron M., & Stott, D. J. (1999). Electrical stimulation of wrist extensors in poststroke hemiplegiaComplete paralysis of the arm, leg, and trunk on one side of the body that results from damage to the parts of the brain that control muscle movements. Hemiplegia is not a progressive condition, nor is it a disease.. StrokeAlso called a "brain attack" and happens when brain cells die because of inadequate blood flow. 20% of cases are a hemorrhage in the brain caused by a rupture or leakage from a blood vessel. 80% of cases are also know as a "schemic stroke", or the formation of a blood clot in a vessel supplying blood to the brain., 30(7), 1384-1389.


